![This is a mini-kidney (1 mm diameter) grown from a patient's stem cells. [Benjamin Freedman & Joseph Bonventre labs]](https://genengnews.com/wp-content/uploads/2018/08/Oct26_2015_BenjaminFreedmanJosephBonventrelabs_MiniKidney2551031276-1.jpg)
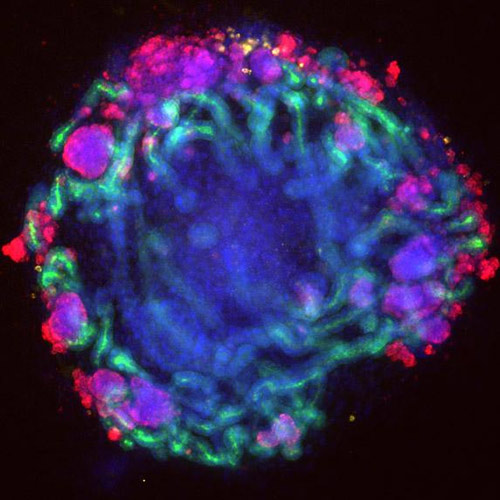
This is a mini-kidney (1 mm diameter) grown from a patient’s stem cells. [Benjamin Freedman & Joseph Bonventre labs]
Kidney-like tissues and even kidney organoids—mini-kidneys—have already been created by means of stem cell choreography. But now some new steps are being introduced. With the addition of genome editing, kidney organoids are showing more promise than ever as disease modeling and drug development platforms.
Mini-kidneys have been grown in a laboratory by properly stimulating human pluripotent stem cells that have also been subjected to the gene-editing technique known as CRISPR. These mini-kidneys, it has been confirmed, are able to recapitulate specific kidney diseases.
This advance was reported October 23 in the journal Nature Communications, in an article entitled, “Modelling kidney disease with CRISPR-mutant kidney organoids derived from human pluripotent epiblast spheroids.” According to this article, the organoids contain tubules, filtering cells, and blood vessel cells. They transport chemicals and respond to toxic injury in ways that are similar to kidney tubules in people.
The study went further, however, demonstrating that genome editing could be applied to create kidney organoids that would model human kidney diseases in a petri dish.
“CRISPR/Cas9 knockout of podocalyxin causes junctional organization defects in podocyte-like cells,” wrote the study’s authors. “Knockout of the polycystic kidney disease genes PKD1 or PKD2 induces cyst formation from kidney tubules. All of these functional phenotypes are distinct from effects in epiblast spheroids, indicating that they are tissue specific.”
Essentially, this work, which was carried out by researchers from Brigham and Women’s Hospital and the University of Washington (UW), resulted engineered mini-kidneys with genetic changes linked to the common kidney diseases polycystic kidney disease and glomerulonephritis.
The organoids developed characteristics of these diseases. Those with mutations in polycystic kidney disease genes formed balloon like, fluid filled sacks, called cysts, from kidney tubules. The organoids with mutations in podocalyxin, a gene linked to glomerulonephritis, lost connections between filtering cells.
“Mutation of a single gene results in changes kidney structures associated with human disease, thereby allowing better understand of the disease and serving as models to develop therapeutic agents to treat these diseases,” explained Joseph Bonventre, M.D., Ph.D., senior author of the study. He is chief of the Renal Division at Brigham and Women's Hospital and a principal faculty member at Harvard Stem Cell Institute.
“These genetically engineered mini-kidneys have taught us that human disease boils down to simple components that can be recreated in a petri dish,” added Benjamin Freedman, Ph.D., the study's lead author and an assistant professor of medicine at UW. “This provides us with faster, better ways to perform 'clinical trials in a dish' to test drugs and therapies that might work in humans.”