![This image shows efficient restoration of OTC expression in the livers of mice treated at neonatal stage by AAV8.CRISPR-SaCas9-mediated gene correction. Immunofluorescence staining with antibodies against OTC on liver sections from an 8-week-old mouse treated with the dual AAV vectors for CRISPR-SaCas9-mediated gene correction as a newborn. [Peter Bell, PhD, Perelman School of Medicine, University of Pennsylvania]](https://genengnews.com/wp-content/uploads/2018/08/107792_web0661211443-1.jpg)
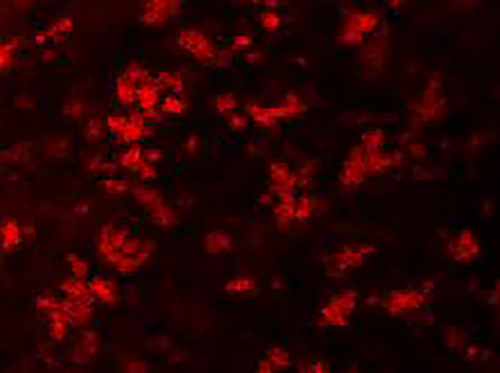
This image shows efficient restoration of OTC expression in the livers of mice treated at neonatal stage by AAV8.CRISPR-SaCas9-mediated gene correction. Immunofluorescence staining with antibodies against OTC on liver sections from an 8-week-old mouse treated with the dual AAV vectors for CRISPR-SaCas9-mediated gene correction as a newborn. [Peter Bell, PhD, Perelman School of Medicine, University of Pennsylvania]
Researchers from the Perelman School of Medicine at the University of Pennsylvania have reached a milestone in the use of genome editing therapy for treating a rare genetic disorder. The Penn team used the adeno-associated virus (AAV) vector to deliver the CRISPR-Cas9 components to newborn mice, improving their survival rate. However, unexpectedly, the treatment of adult mice actually worsened their symptoms.
“Correcting a disease-causing mutation following birth in this animal model brings us one step closer to realizing the potential of personalized medicine,” explained senior study author James Wilson, M.D., Ph.D., professor of medicine and director of the Orphan Disease Center at Penn. “Nevertheless, my 35-year career in gene therapy has taught me how difficult translating mouse studies to successful human treatments can be. From this study, we are now adjusting the gene-editing system in the next phases of our investigation to address the unforeseen complications seen in adult animals.”
The findings from this study were published recently in Nature Biotechnology through an article entitled “A dual AAV system enables the Cas9-mediated correction of a metabolic liver disease in newborn mice.”
Dr. Wilson’s laboratory had previously used traditional gene therapy vectors based on AAV for various other liver disorders. Gene replacement therapy with AAV is not ideal, however, for treating genetic diseases of the liver that manifest as newborns because the non-integrating genome is lost as developing liver cells proliferate. Thus, investigators decided to utilize an AAV-mediated gene correction system using CRISPR-Cas9.
The researchers tested their hypothesis in a mouse model of a rare metabolic urea cycle disorder caused by a deficiency in an enzyme called ornithine transcarbamylase (OTC). The urea cycle is a series of six liver enzymes that help rid the body of ammonia, a breakdown product of protein metabolism. When one of these enzymes is missing or deficient, ammonia accumulates in the blood and travels to the brain, typically causing a multitude of problems, including brain damage and death. OTC deficiency is the most common of the urea cycle disorders, occurring in one out of every 40,000 births. A mutated OTC gene can cause an enzyme that is shorter than normal, the wrong shape, or may not be produced at all.
The researchers injected two AAVs (specifically an AAV8 serotype they discovered previously that has an affinity for liver cells), one expressing Cas9 and the other expressing a guide RNA and a donor DNA, into newborn mice with OTC deficiency.
The Penn team tried to limit any off-target activity by using a liver-specific promoter for Cas9, ensuring its expression only within liver cells. The second AAV injected carried a guide RNA 20 base pairs in length followed by another sequence to lead the Cas9 enzyme to the correct spot in the genome. Moreover, the second AAV also contained a donor DNA template to correct the mutation so that the normal OTC protein can be made by the cell. The use of donor DNA for correcting a mutation differentiates this study from other recent genome-editing research findings, which circumvent a mutation by deleting a portion of the normal gene.
The investigators noted that the whole correction system was a “cut-and-paste” function, with the last part of the “paste” phase relying on the cells' own DNA repair mechanism to properly join the OTC gene back together again.
The newborn mice tolerated the AAV therapy well and even entirely reversed the OTC mutation in up to 10% of the treated animals. In adult mice (8–10 weeks), symptoms worsened.
“We were surprised by these results, but after some further investigation, we deciphered the mechanism by which gene editing worsened the condition of the adult animals,” noted Lili Wang, Ph.D., research associate professor of pathology and laboratory medicine at Penn. Looking at the DNA sequence in liver cells in adult mice, they found that the frequency of cells that had a corrected “paste” function was only about one percent. “This was certainly not enough to help these adult mice,” Dr. Wang added.
The researchers found that in newborns, the cut and paste system is mediated by homology-directed DNA repair, whereas in adult animals, the process was completed by non-homologous end joining (NHEJ), which leaves in its wake small insertions or deletions.
“It appears that HDR is more efficient in newborn liver cells than in adult liver cells.” Dr. Wilson remarked. “The untoward consequences of gene editing observed in adult OTC mice is limited to treating genetic diseases in which the mutation diminishes but does not eliminate function.”
Looking toward the future, Dr. Wilson and his colleagues are trying to avoid this problem by exploring methods to create the “cut” without inciting the large deletions while at the same time, driving higher frequencies of the “paste.”