Chimeric antigen receptor (CAR) T cells are about as cutting-edge as cancer care gets today. Having demonstrated the ability to eradicate tumor cells in up to 90% of patients1 with certain blood cancers, these engineered immune cells became the first class of gene therapy to win FDA approval in 2017—with Novartis’ Kymriah getting the nod in August,2 followed by Kite Therapeutics’ Yescarta in October.3 But Alexander Marson, MD, PhD, knows these sophisticated cells are capable of so much more.
Marson, an immunologist at the University of California at San Francisco, is exploring this potential by using the CRISPR-Cas9 system to introduce precisely targeted genome modifications. The idea is that by adding or deleting specific genomic sequences, one can make these cells more lethal for tumors but also safer for the patient. Marson’s team recently developed a platform called SLICE4—single-guide RNA (sgRNA) lentiviral infection with Cas9 protein electroporation—to perform diverse CRISPR modifications in many cells in parallel, in hopes of rapidly identifying changes that measurably improve CAR T-cell performance. “We’re pretty good at manufacturing the ‘hardware’ of gene edited cells, and we’re continuing to improve that,” says Marson. “The really interesting thing will be what genetic ‘software’ we can put into them.”
Targeted tweaks for sturdier cells
This question has intrigued many in the immunotherapy space, and the advent of robust genome editing technologies has greatly simplified the pursuit of answers. Michel Sadelain, MD, PhD, an immunologist at the Memorial Sloan-Kettering Cancer Center, recalls strong skepticism when he began working on T-cell engineering 30 years ago. “Most people found the idea to be bizarre if not laughable,” he recalls. “It took me three years to figure out how to put a gene into about 0.5% of a batch of T cells, and we were celebrating when we saw that!” Such genetic modification has now become routine, and multiple pharmaceutical companies are now efficiently producing the CAR T-cell therapies pioneered by Sadelain and Carl June, MD, professor in immunotherapy in the department of pathology and laboratory medicine at the University of Pennsylvania (UPenn), at clinical scale.
The reprogramming of T cells to express tumor-specific CARs is currently performed with the same virus-based genome manipulation strategies that have been in use for many years. But CRISPR offers an appealing alternative to this laborious and imprecise process, giving researchers the opportunity to rapidly prototype and test a variety of targeted genetic modifications to see which has the desired effect. “Any lab can relatively easily generate CRISPR reagents, and you can do CRISPR modification in a few days to a week,” says Waseem Qasim, PhD, a gene therapy specialist at University College London. Armed with these capabilities, researchers are finding abundant opportunities to begin tackling the limitations of CAR T-cell therapy.
From a logistical perspective, one of the biggest challenges with CAR T cells is the need to whip up a fresh batch for each new patient. This creates additional costs and delays, but is essential to avoid the risk of potentially lethal immune rejection that can arise following transplantation from an imperfectly matched donor. Qasim and colleagues have taken an important step toward off-the-shelf “universal” CAR T cells by using genome editing to selectively ablate the native T-cell receptor (TCR) in donor cells, essentially eliminating the sensory organ that allows T cells to recognize and attack threats—or in this context, initiate damaging graft-versus-host disease.
As a result, these cells only go after targets recognized by the CAR. His team initially demonstrated this approach with an older editing technology known as TALENs and obtained encouraging results—early data from a trial for leukemia5 indicate that these cells put 88% of patients into remission with only a minority experiencing some modest toxicity. Qasim’s group is now pursuing similar efforts with CRISPR. “We’re expecting to have some of these projects ready for trials in 2019,” he says.

A similar engineered T-cell effort represents the first-ever use of CRISPR in a U.S. clinical trial.6 Yangbing Zhao, MD, PhD, Edward Stadtmauer, MD, and colleagues at UPenn selectively deleted a key component of the TCR from donor T cells while also introducing an engineered TCR construct that recognizes a tumor antigen known as NY-ESO-1.7 In addition to potentially eliminating graft-versus-host toxicity, this modification greatly improves the performance of the engineered cells by preventing inappropriate interactions between natural and engineered receptor proteins. “Mispairing can cause some specificity issues, which in mouse models can even be occasionally lethal,” says Zhao.
Sadelain’s team has found a way to exploit CRISPR to make an off-the-shelf therapy that also delivers a far more potent response to boot. One major limitation of virus-based genome modification is that foreign genes are essentially randomly slotted into the genome, and the resulting context can profoundly affect gene activity. “This means in some cells it will be expressed really high, in some cells really low, and in some not at all,” says Sadelain, noting that the variability in the resulting batches of cells means that higher doses must be administered to better ensure efficacy.
To resolve this, his team used CRISPR to directly swap out the native TCR gene in donor T cells with an engineered CAR gene,8 eliminating a key risk of rejection while also putting the foreign receptor in a strong position for naturalistic expression. The resulting cells achieved consistent CAR expression and delivered dramatically stronger and longer-lasting antitumor activity in a mouse model of leukemia, and Sadelain is excited about the prospect of achieving more benefit with less treatment. “If the dose is lower, we predict it should also reduce toxicities,” he notes.
One can also unleash the power of CARs by releasing the natural brakes on immune response. The same cell-signaling pathways targeted by the various blockbuster “checkpoint inhibitor” drugs can also be manipulated in CAR T cells to allow them to operate unfettered, even in the highly immunosuppressive milieu of solid tumors—a class of malignancies that have proven challenging for CAR T-cell therapy. “We used a CAR in a mouse prostate cancer model and found that this PD-1 knockout improved the CAR T-cell treatment,” reports Zhao. His team will also be knocking out this checkpoint protein in the T cells used for an upcoming clinical trial.7,9
The next chapter for clinical CRISPR
Several other trials are now in the works, and in many ways, the CAR T-cell platform is an ideal vehicle for introducing CRISPR into the clinic. Primary T cells can now undergo CRISPR editing with efficiencies of 50–80% depending on the specific method employed, and many groups now achieve targeted manipulation of up to three different loci in parallel without dragging down the overall efficiency. Furthermore, since the modification is done in a lab setting rather than in vivo, the likelihood of unintended consequences is low, and there is little evidence that editing might unwittingly inflict potentially tumorigenic damage through off-target effects. “T cells are very stable and difficult to transform,” assures Zhao.
But techniques that work in the laboratory may not scale well or meet the rigors of clinical testing. “We’ve got to put in the bells and whistles for the safety aspects,” says Qasim of his clinical development efforts, which include the use of RNA encoding the Cas9 enzyme rather than a Cas9 gene that could stick around indefinitely and increase the risk of off-target cuts over time. “We don’t think the Cas9 is around for more than a week,” he says. As an alternative, Marson uses a system developed in collaboration with Jennifer Doudna, PhD, at the University of California at Berkeley, one of the researchers who first established the CRISPR-Cas9 editing technique. This entails preloading the Cas9 protein with the guide RNA that targets the CRISPR editing process, and then using electroporation to deliver these complexes into cells.10
“It gets delivered and makes a permanent genetic modification, but the Cas9 protein should be diluted or degraded over time,” says Marson. His team has also devised an approach that eliminates the need for viral vectors to deliver the CAR gene, eliminating a major source of manufacturing costs and delays.11 “All of these components should be readily adaptable for GMP clinical-grade manufacturing of these cells,” he maintains.
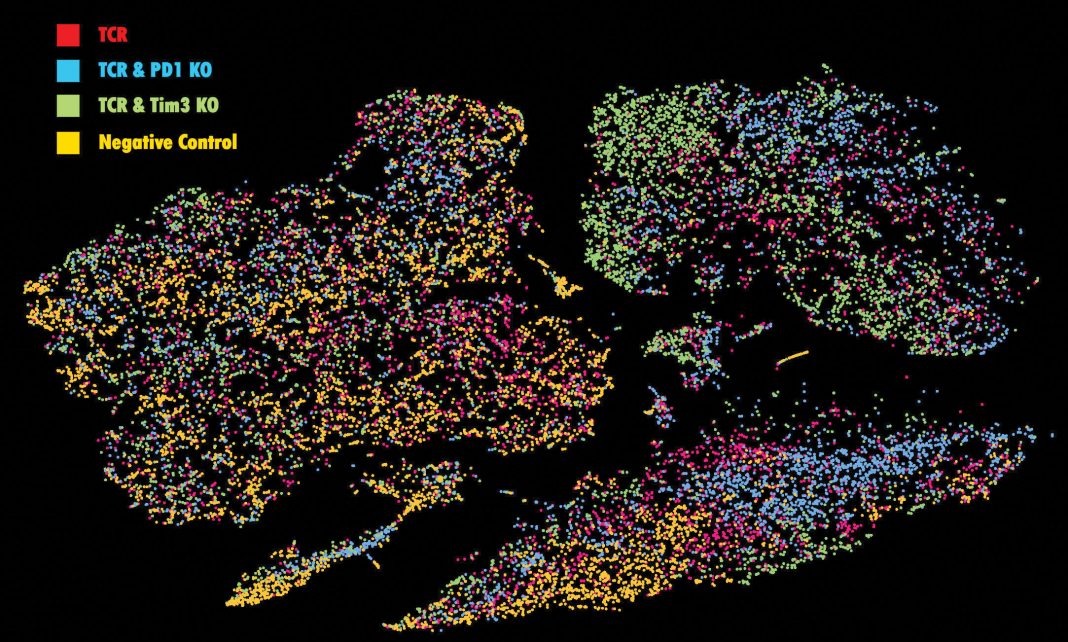
The electroporation procedure also enabled Marson and colleagues to perform a wide array of genome modifications in a massively parallel fashion in their recently published SLICE platform.4 They generated guide RNAs targeting more than 19,000 different genes, which they introduced into donor human T cells with a retrovirus to enable stable expression. After electroporating the cells with Cas9 protein to achieve a brief flurry of editing, they were left with a vast library of modified T cells, which could then be assessed for functional changes. “We used that to screen for gene knockouts that boost T-cell proliferation or make cells resistant to adenosine immunosuppression, which we know is an important factor in limiting T-cell function,” says Marson. This initial study revealed at least four candidate genes that could potentially be manipulated in next-generation CAR T cells to deliver better performance.
Such screens will give scientists greater opportunities to tinker with and decipher the regulatory circuitry of immune cells. The resulting findings will imbue greater confidence in clinicians and regulators as engineered T cells become more commonplace, but could also lay a foundation for more ambitious rewiring efforts. For example, Zhao sees the potential for T cells to act as medics rather than assassins. “You could modify T cells to specifically target some site in the body, and then make a drug and deliver it at those sites,” he suggests. This potential also excites Marson, who wants more biologists to give in to their inner hacker. “We hope that there’s really a broad base of inventors who start writing the equivalent of genetic ‘apps,’” he says.
Michael Eisenstein ([email protected]) is a freelance science writer and photographer.
Resources
1. www.nejm.org/doi/10.1056/NEJMoa1709919
2. www.fda.gov/newsevents/newsroom/pressannouncements/ucm574058.htm
3. www.fda.gov/newsevents/newsroom/pressannouncements/ucm581216.htm
4. www.cell.com/cell/fulltext/S0092-8674(18)31333-3
5. ash.confex.com/ash/2018/webprogram/Paper111356.html
6. www.nature.com/news/first-crispr-clinical-trial-gets-green-light-from-us-panel-1.20137
7. clinicaltrials.gov/ct2/show/NCT03399448
8. www.nature.com/articles/nature21405
9. clincancerres.aacrjournals.org/content/23/9/2255.long
10. www.pnas.org/content/112/33/10437.long
11. www.nature.com/articles/s41586-018-0326-5