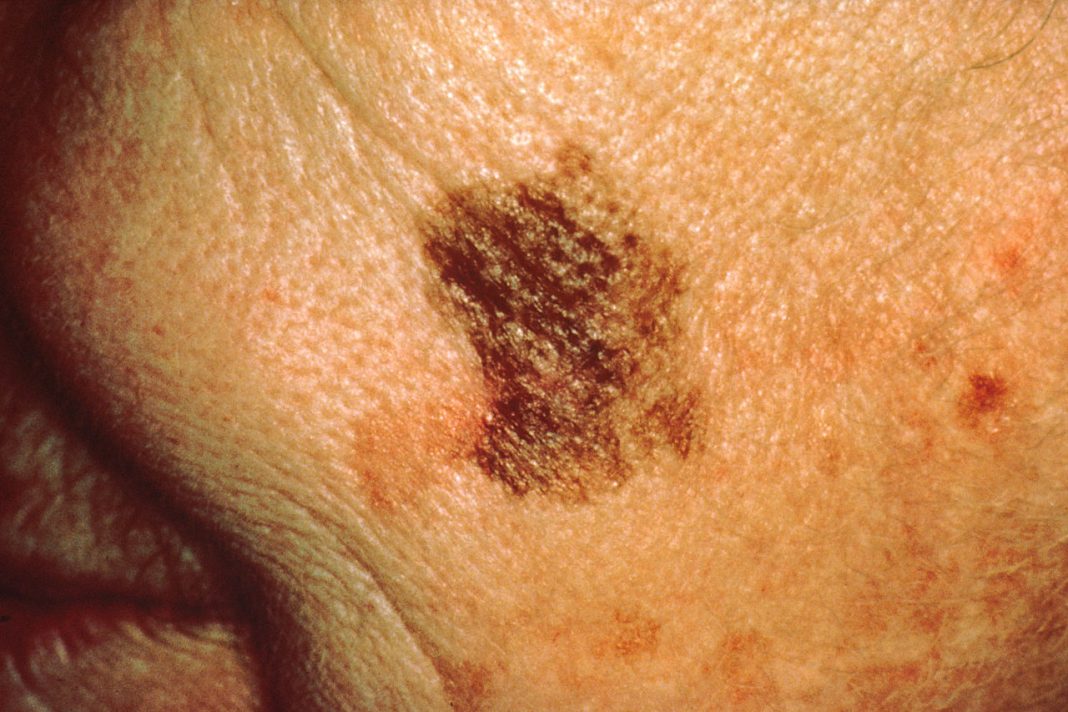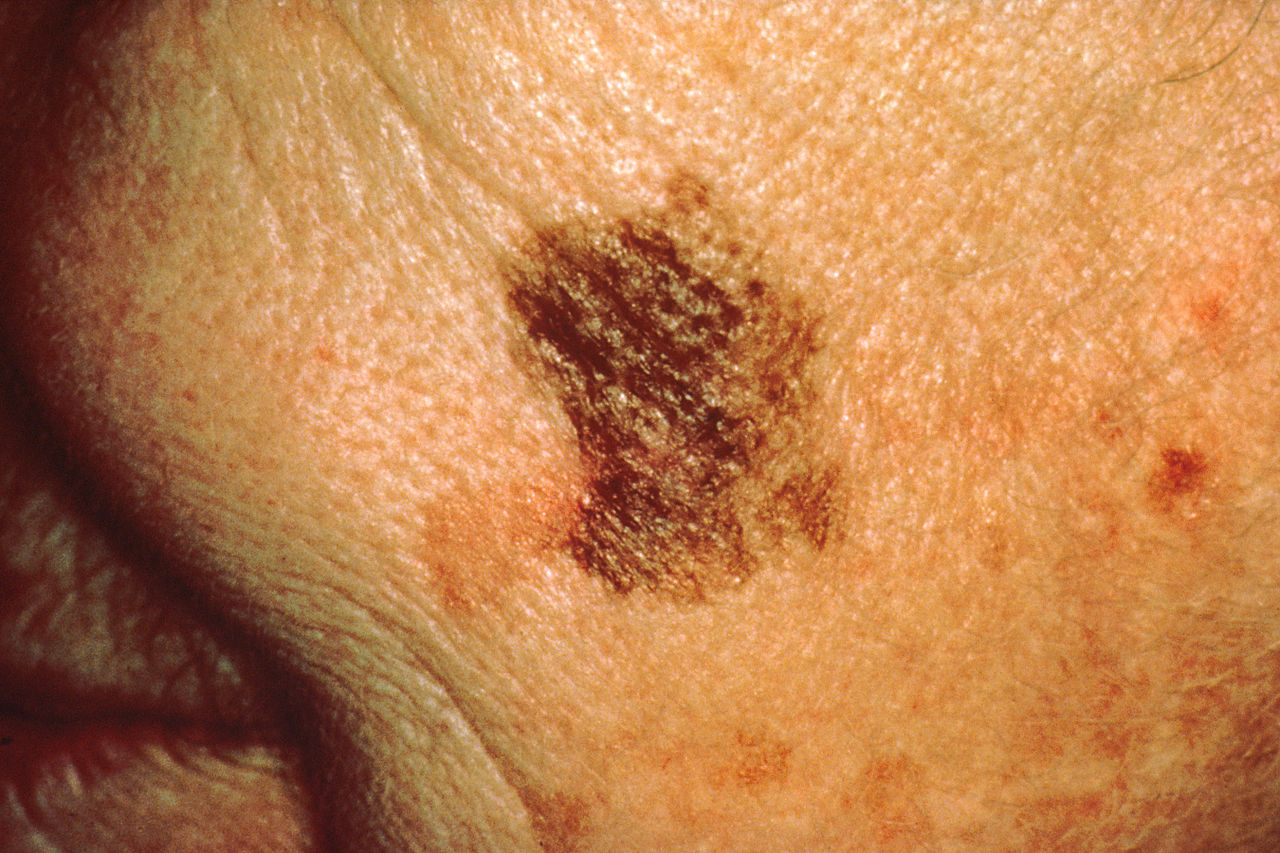
Source: Wikipedia
Obese men with metastatic melanoma who are treated using targeted or immuno-therapies survive for more than twice as long as patients receiving the same treatment, but who have a normal body mass index (BMI), according to a retrospective study by researchers at the University of Texas MD Anderson Cancer Center. Their analysis of independent cohorts of metastatic melanoma patients found that the survival-boosting effects of obesity didn’t extend to female patients, nor was obesity associated with increased survival in men receiving chemotherapy.
“Obese men consistently did much better than men with a normal BMI, with nearly a doubling of overall survival,” comments Jennifer McQuade, M.D., lead author of the team’s published paper in Lancet Oncology, and instructor of melanoma medical oncology at the University of Texas MD Anderson Cancer Center. However, McQuade stresses, “The public health message is not that obesity is good. Obesity is a proven risk factor for many diseases. Even within our metastatic melanoma population, we would not suggest that patients intentionally gain weight. We need to figure out what is driving this paradox and learn how to use this information to benefit all of our patients.”
Obesity is a well recognized risk factor for many types of cancer, and is associated with worse outcomes in patients with several tumor types, Dr. McQuade and colleagues write in their published study, “Association of body-mass index and outcomes in patients with metastatic melanoma treated with targeted therapy, immunotherapy, or chemotherapy: a retrospective, multicohort analysis”. However, a high BMI has also been associated with improved outcomes in some cancers, a phenomenon that has been dubbed the “obesity paradox.”
Although the role of obesity in melanoma hasn’t been investigated in depth, existing data does indicate that obesity is associated with an increased risk of melanoma in men. Recent research by the MD Anderson team also reported that higher BMI is associated with worse survival in patients with surgically resected melanoma. And while any association between BMI and survival outcomes in patients with metastatic melanoma—and in particular in those treated using the most recent targeted and immunotherapies—has yet to be identified, existing evidence appears to be stacking up to suggest that obesity might be associated with poorer prognosis.
“Notably, several associations have been described that could link obesity with worse survival outcomes in patients with melanoma, including germline genetic variants in obesity-related genes associated with melanoma risk, inflammation, obesity-related cytokines, and pro-tumorigenic adipocyte cross-talk,” the researchers comment.
Prior studies have linked the IGF1/PI3K/AKT pathway with obesity-related pathogenesis in cancer, and this pathway has also been implicated in resistance to both targeted and immuno-therapies in melanoma, the authors note. Based on these findings, the researchers’ initial hypothesis was that “obesity would be associated with worse outcomes in patients with metastatic melanoma.” They set out to investigate any possible link between BMI and patient outcomes by analyzing data from six existing clinical cohorts of metastatic patients, including 1,918 individuals who had been treated using different types of therapy.
“We assessed the association of BMI with progression-free survival and overall survival in independent cohorts of patients with metastatic melanoma treated with targeted therapy, immunotherapy, or chemotherapy,” they write. “Because of the well-documented sex disparity in melanoma outcomes, as well as sex differences in body composition, we examined associations in male and female patients separately.”
The results threw up some surprises. It has long been known that, unrelated to obesity, women with metastatic melanoma have better outcomes than men, but the MD Anderson study results showed that obesity gave men an even greater survival advantage, dependent upon the type of treatment they received. Obesity was associated with both increased progression-free survival (PFS) and significantly increased overall survival (OS) in male metastatic melanoma patients who were treated using targeted and immuno-therapies, but not among men who were treated using chemotherapy.
PFS and OS among men with normal BMI who were treated using combination-targeted therapy comprising dabrafenib (a BRAF inhibitor) and trametinib (an MEK inhibitor) were 7.2 months and 16.0 months, respectively. For obese men receiving the same treatments, PFS and OS were 12.8 months and 36.5 months, respectively. Overall survival for women was at least 33 months, irrespective of BMI. An evaluation of data from a validation cohort of another 240 patients treated using vemurafenib (a BRAF inhibitor) and cobimetinib (an MEK inhibitor) generated similar results.
The relationship between BMI, immunotherapy and survival again indicated no differences among women. However, obesity among men treated using immunotherapy was linked with significantly improved OS. For men with normal BMI, PFS and OS were 2.7 months and 14.3 months, respectively, following treatment with either a PD1 checkpoint inhibitor or PD-L1 inhibitor. PFS and OS were much higher in obese men receiving the same immunotherapies, at 7.6 months and 26.9 months, respectively. Similar results were obtained in a validation cohort of 207 patients treated using the immune checkpoint inhibitor ipilimumab.
“Our analysis showed that obesity was associated with improved survival in metastatic melanoma, an association that, to our knowledge, has not been identified previously,” the researchers claim. “These associations seemed to be independent of traditional prognostic factors and concomitant medications, and were not explained by differences in treatment tolerance or pharmacokinetics.”
Interestingly, for other cancers in which an obesity paradox has been reported, the survival advantage tends to be limited to patients who are overweight or only mildly obese. In contrast, data from the MD Anderson study suggest that in metastatic melanoma there is a dose-related effect of BMI, such that the survival advantage increases with increasing BMI. “We also observed a nearly linear association between increasing BMI and PFS that extended to morbid obesity (where body composition is unlikely to be misclassified) in the dabrafenib plus trametinib cohort,” they state. “These results have implications for the design of future clinical trials for patients with metastatic melanoma and the magnitude of the benefit found supports further investigation of the underlying mechanism of these associations.”
“The question is: What underlying mechanism causes this advantage in obese men, and can we take advantage of it to improve outcomes in patients with melanoma?” Dr. McQuade notes. “One hint may be the interaction between obesity, sex, and outcomes, which has not been detected before in any cancer.”
The differential effects of BMI on survival according to sex points toward the possibility that a hormonal mechanism is at work. In men, aromatase enzyme in adipose tissue converts androgens to estrogen compounds, resulting in higher circulating levels of estradiols. Dr. McQuade’s team is now working with investigators at the University of Pennsylvania, who have found that turning on a particular estrogen receptor on melanoma cells makes them vulnerable to immunotherapy. The MD Anderson team is also looking at gene expression, mutations and immune profiling to identify possible differences in melanoma between obese and non-obese patients, and developing preclinical models. “The association of BMI and outcomes in other malignancies in which targeted or immuno-therapies are approved should also be examined,” they state.