Patricia F. Fitzpatrick Dimond Ph.D. Technical Editor of Clinical OMICs President of BioInsight Communications
This first part of a two-part article on treating Duchenne muscular dystrophy focuses on a potential new treatment that interferes with nonsense mutations.
Using genetic editing, Duke University scientists reported this month that they had repaired a genetic defect responsible for Duchenne muscular dystrophy (DMD) in patient cell samples. While still in preclinical development, the approach may offer a giant step forward in the treatment of certain genetic diseases.
Conceptually, manipulating a gene product at either the DNA level through editing to restore production of a functional protein, or at the translational level by preventing production of a dysfunctional gene product, could provide the means to treat other genetic diseases caused by a few gene mutations, such as cystic fibrosis and other muscular dystrophies.
This first segment of a two-part article discussing therapeutic approaches to treating this disease focuses on interfering with nonsense mutations that result in the production of inactive dystrophin protein.
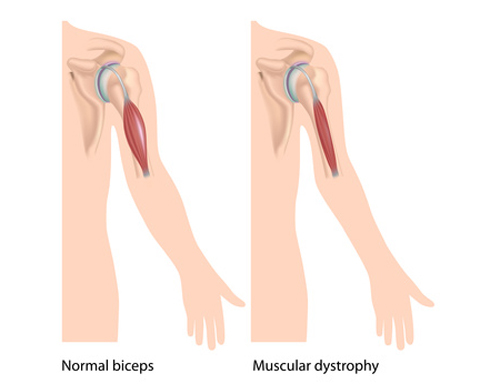
DMD, an X-chromosome-linked genetic disease, occurs when one of several types of mutations in the dystrophin gene prevent production of a functional dystrophin protein, essential for maintaining structural integrity of muscle fibers. The disease affects one in 3,600 newborn males; individuals with the disorder suffer gradual muscle deterioration, eventually resulting in paralysis and death, usually by age 25.
With few exceptions, scientists say, all DMD mutations, deletions, and duplications lead to frame shifts, resulting in the formation of a premature termination codon that impairs translation of mRNA into functional dystrophin. When mutations do not perturb the correct reading frame, as in the case of Becker muscular dystrophy (BMD), the translation of a partially functional protein occurs. BMD patients carrying deletions of about half of the DMD gene show very mild symptoms.
There is currently no marketed therapy approved for the treatment of the underlying cause of Duchenne muscular dystrophy, but many companies are testing potential candidates aimed at either adding new genetic material to compensate or “override” the faulty gene, or interfering with the protein synthesis of a faulty protein. A completely novel approach to treating this disease has emerged from post-transcriptional control processes.
PTC Therapeutics says it applies its proprietary technologies and knowledge of post-transcriptional control processes to its drug discovery and development activities. The company reports that its scientists discovered its lead product candidate (ataluren) by applying its technologies to identify molecules that promote or enhance the suppression of nonsense mutations.
A Good-Enough Partial Protein that Works
Ataluren, intended for the treatment of patients with genetic disorders arising from a nonsense mutation, is a small molecule drug, and has the potential, the company says, to overcome the effects of a nonsense mutation and allow production of functional dystrophin.
During translation of mRNA into protein in healthy individuals, ribosomes keep going until arriving at a normal stop signal in the mRNA, at which point the ribosome appropriately ceases translation and a functioning protein results.
Nonsense mutations, however, promote premature translational termination—causing anywhere from 5–70% of individual cases of most inherited diseases—by creating a premature stop signal in the mRNA causing the ribosome to stop translation before a functioning protein is generated, creating a shortened, nonfunctioning protein.
The resulting disease is determined by which protein cannot be expressed in its entirety and is no longer functional. Specifically, nonsense mutations give rise to in-frame UAA, UAG, or UGA stop codons in the mRNA coding region, leading to premature translational termination and truncated protein products. Based on information from Prior, et al. (1995) in the American Journal of Human Genetics, PTC estimates that a nonsense mutation is the cause of Duchenne muscular dystrophy in approximately 13% of patients, or 2,000 patients in the U.S. and 2,500 patients in the European Union.
PTC’s therapeutic strategy, based on discoveries by its own scientists and from researchers in the department of physiology, University of Pennsylvania School of Medicine, and the department of molecular genetics and microbiology, University of Massachusetts Medical School, was to discover a drug capable of suppressing premature termination. The scientists identified a small molecule, PTC124, that selectively induces ribosomal read-through of premature, but not normal, termination codons. Two high-throughput screens (comprising ~800,000 low molecular weight compounds) were performed to identify compounds that promoted UGA nonsense suppression.
PTC124 activity, optimized using nonsense-containing reporters, promoted dystrophin production in primary muscle cells from humans and mdx mice, a model of Duchenne muscular dystrophy (mice expressing dystrophin nonsense alleles), and rescued striated muscle function in mdx mice within 2–8 weeks of drug exposure.
In short, ataluren acts, the company believes, by interacting with the ribosome, enabling it to read through premature nonsense stop signals on mRNA, and allowing the cell to produce a full-length, functional protein. The company says that that the small molecule drug has the potential to treat other genetic disorders for which a nonsense mutation is the cause of the disease.
In June 2012, the company announced the initiation of an open-label study in the European Union, Israel, Australia, and Canada for patients with nonsense mutation Duchenne/Becker muscular dystrophy (nmDBMD) and who had received ataluren in a prior, PTC-sponsored clinical study. The new study aims to gain further information on the long-term safety and tolerability of the drug.
PTC launched a similar study in the U.S. in November 2010. The initial results of the international Phase IIb clinical trial of ataluren showed that the lower of the two doses tested was more beneficial than the higher dose, and because of this unexpected outcome all ongoing studies had been halted in April 2010. In the U.S. all boys with Duchenne who participated in the Phase IIb study have been receiving the lower dose in an extension trial since November 2010.
“The initiation of this open-label study is based on the potential ataluren has shown in previous studies in nonsense mutation Duchenne/Becker muscular dystrophy,” stated Stuart W. Peltz, Ph.D., CEO of PTC Therapeutics. “We are encouraged by the results we have obtained in our Phase IIb study and are committed to the continued advancement of the development of ataluren.”
PTC has initiated a Phase III confirmatory trial of ataluren in patients with nonsense mutation Duchenne muscular dystrophy (nmDMD). The European Medicines Agency, or EMA, has designated ataluren as an orphan medicinal product, and the U.S. Food and Drug Administration, or FDA, has granted orphan drug designation to ataluren for the treatment of both nmDMD and nmCF.
The company said, in its recent S-1 filing with the SEC, that it had dosed the first patient in its nmDMD trial in April 2013. The company also submitted a marketing authorization application, or MAA, to the EMA for conditional approval of ataluren for the treatment of nmDMD.
In March this year, PTC announced the completion of a $60 million financing led by Brookside Capital Partners Fund. Joining Brookside as new investors in this financing are Adage Capital Management, Jennison Associates, Longwood Fund, and additional institutional investors.
Proceeds from the financing, the company says, will support continued clinical development of ataluren in Duchenne and cystic fibrosis.
While this therapeutic approach may prove helpful with about 13% of patients with the mutation that will potentially be compensated for by the drug, other patients with a host of other mutations in the dystrophin gene will require other therapies. Some of these will be discussed in part 2 of this article.
Patricia Fitzpatrick Dimond, Ph.D. ([email protected]), is technical editor at Genetic Engineering & Biotechnology News.