Researchers have reduced the formation and growth of kidney cysts in autosomal dominant polycystic kidney disease (ADPKD) models by blocking the binding of a microRNA called miR-17 to the PKD1 and PKD2 transcripts. The findings pave the way for a therapeutic strategy with the potential to arrest or cure ADPKD.
“For more than 25 years, we have known that ADPKD is caused by mutations of PKD1 or PKD2 genes. Yet, no therapeutic strategy exists to go after these root causes,” said Vishal Patel, MD, associate professor of internal medicine in the division of nephrology at UT Southwestern. Patel’s team led the work, which was published in Nature Communications in an article entitled “PKD1 and PKD2 mRNA cis-inhibition drives polycystic kidney disease progression.”
ADPKD is among the most common human genetic conditions and the most frequent genetic cause of kidney failure, affecting an estimated 12.5 million people worldwide. Patients have one mutated copy of PKD1 (or PKD2) and one normal copy.
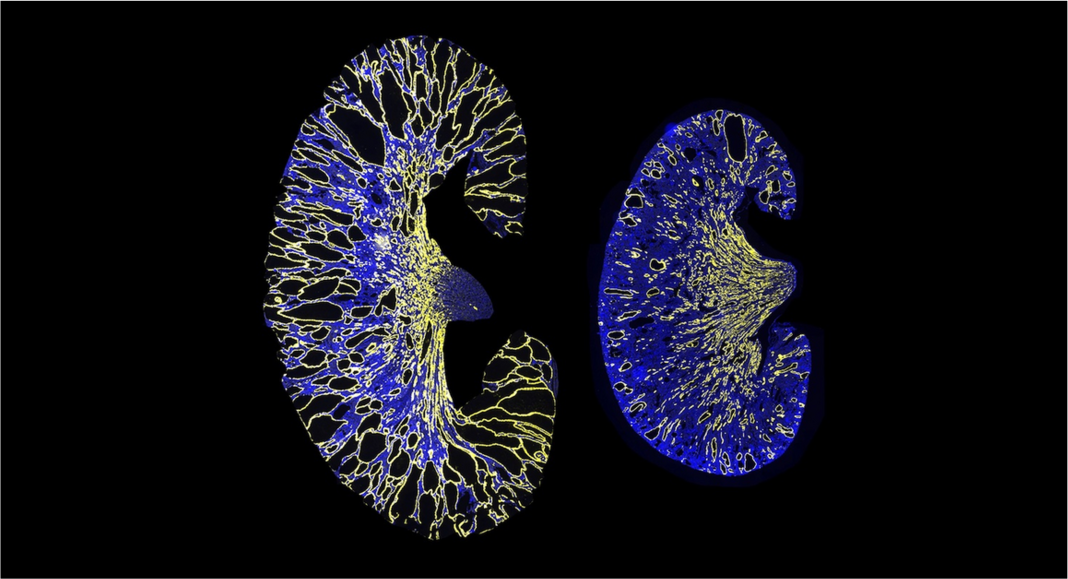
The disease is characterized by the formation of many small fluid-filled cysts. In recent years, scientists have begun to think that these cysts form when the levels of PKD1 or PKD2 expression fall below a critical threshold—in other words, when the normal copy of the gene does not produce enough of the corresponding protein Polycystin-1 or Polycystin-2.
“[I]f reduced dosage causes ADPKD, increasing the expression of the normal PKD1 allele could arrest the disorder,” wrote the investigators in the article. “However, despite this transformative potential, the factors governing PKD1 dosage in ADPKD are mostly unknown, and currently, there are no mechanisms to activate the normal PKD1 allele.”
PKD1 mRNA contains a binding site for miR-17, a microRNA that is highly expressed and active in models of ADPKD. The miR-17 binding site is in the 3’-UTR of the mRNA, a region of code that helps protect the mRNA from degradation but can also control how much of the protein is made.
With this in mind, Patel and his colleagues asked if blocking the binding of miR-17 to PKD1 could prevent kidney cyst formation.
“We use CRISPR/Cas9 editing to delete the miR-17 motif from the PKD1 gene in monoallelic ADPKD models,” they wrote. “We find that eliminating the miR-17 motif is sufficient to improve Pkd1 mRNA stability, raise Polycystin-1 (PC1) expression, and ameliorate cyst growth in cellular, ex vivo, and mouse PKD models.
“The other ADPKD gene, PKD2, also contains a 3′-UTR miR-17 binding motif,” they continued, “remarkably, deleting this miR-17 motif increases Polycystin-2 (PC2) levels and attenuates cyst growth in Pkd1-mutant models.”
Moreover, the group found that blocking miR-17 binding to PKD1 mRNA with the anti-miR-17 drug RGLS4326 after cyst formation also decreased cyst growth, indicating that this interaction could be a promising target for polycystic kidney disease (PKD) treatment.
“On a cautionary note,” the researchers wrote, “raising Pkd1 above wildtype levels produces cystic disease in mice. However, the uniqueness of our method is that, rather than transactivation, it relies on preventing inhibition, making it unlikely that PKD1 will rise to the supratherapeutic range.”
Patel has patents involving anti-miR-17 for the treatment of ADPKD and serves as a scientific consultant for Regulus Therapeutics and other companies as disclosed in the paper.
“There are numerous genetic conditions where one copy of the causative gene is mutated, but the other copy is still normal,” Patel said. “Our approach to harnessing the remaining normal copy is likely applicable to many other diseases besides PKD.”