![Stem cell-derived photoreceptor cells injected into the retina improved eyesight. [University of Toronto]](https://genengnews.com/wp-content/uploads/2018/08/May15_2015_UnivToronto_StemCellDerivedPhotoreceptorCells5744369354-1.jpg)
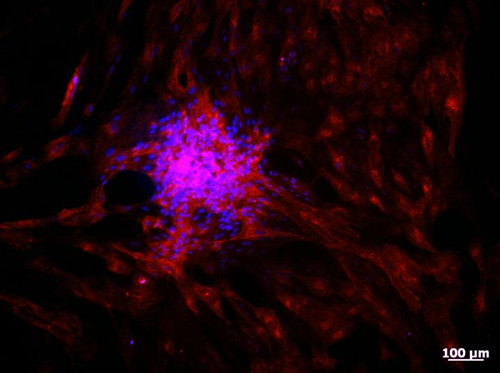
Stem cell-derived photoreceptor cells injected into the retina improved eyesight. [University of Toronto]
University of Toronto (U of T) scientists say they have made a breakthrough in cell transplantation using a gel-like biomaterial that keeps stem cells alive and helps them integrate better into tissue. In two early lab trials, they note that their approach has already shown to partially reverse blindness and help the brain recover from stroke.
Molly Shoichet, Ph.D., and colleagues encased stem cells in a hydrogel that reportedly boosted their healing abilities when transplanted into both the eye and the brain. Conducted through the University of Toronto’s Donnelly Center for Cellular and Biomolecular Research, the group’s study (“A Hyaluronan-Based Injectable Hydrogel Improves the Survival and Integration of Stem Cell Progeny following Transplantation”) was published in Stem Cell Reports.
Dr. Shoichet, a bioengineer who recently won the L'Oreal-UNESCO for Women in Science Award, and her team created the hydrogel several years ago as a kind of a bubble wrap to hold cells together during transport and delivery into a transplant site.
“This study goes one step further, showing that the hydrogels do more than just hold stem cells together; they directly promote stem cell survival and integration. This brings stem-cell based therapy closer to reality” says Dr. Shoichet, a professor whose affiliations span the Donnelly Center, the department of chemical engineering and applied chemistry and the Institute of Biomaterials and Biomedical Engineering at U of T.
In addition to examining how the stem cells benefit from life in hydrogels, the researchers also showed that these new cells could help restore function that was lost due to damage or disease. One part of the study involved the team injecting hydrogel-encapsulated photoreceptors, grown from stem cells, into the eyes of blind mice. Photoreceptors are the light sensing cells responsible for vision in the eye. With increased cell survival and integration in the stem cells, they were able to partially restore vision.
“After cell transplantation, our measurements showed that mice with previously no visual function regained approximately 15% of their pupillary response. Their eyes are beginning to detect light and respond appropriately,” explains Brian Ballios, Ph.D., an expert in stem cell biology and regenerative medicine for retinal degenerative disease, who led this part of the study.
In another part of the study, Michael Cooke, Ph.D., a postdoctoral fellow, injected the stem cells into the brains of mice who had recently suffered strokes.
“After transplantation, within weeks we started seeing improvements in the mice's motor coordination,” says Dr. Cooke. His team now wants to carry out similar experiments in larger animals, such as rats, who have larger brains that are better suited for behavioral tests, to further investigate how stem cell transplants can help heal a stroke injury.
According to Dr. Shoichet, because the hydrogel could boost cell survival in two different parts of the nervous system, the eye and the brain, it could potentially be used in transplants across many different body sites. Another advantage of the hydrogel is that, once it has delivered cells to a desired place, it dissolves and is reabsorbed by the body within a few weeks.