![GLT-1, a glutamate transporter, soaks up glutamate (a neurotransmitter) released by neurons and converts it back into a safer substance. [Wilson lab, UC Riverside]](https://genengnews.com/wp-content/uploads/2018/08/117047_web1018523716-1.jpg)
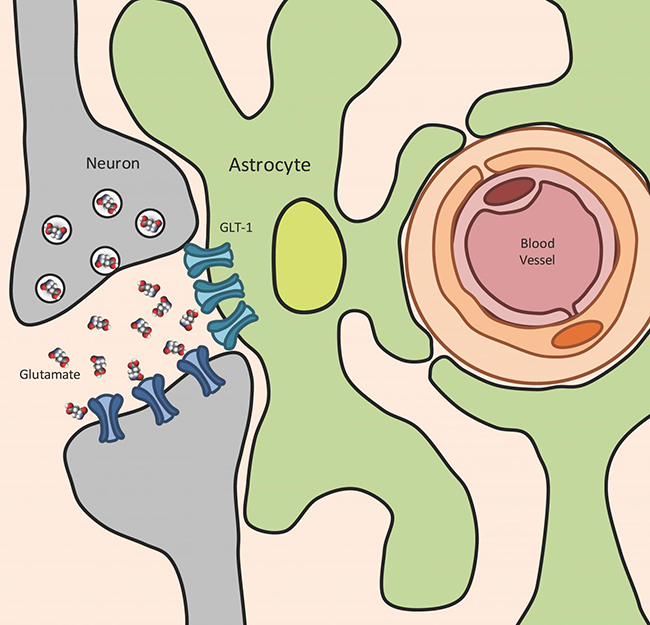
GLT-1, a glutamate transporter, soaks up glutamate (a neurotransmitter) released by neurons and converts it back into a safer substance. [Wilson lab, UC Riverside]
A cold shudder would radiate down most anyone’s spine when thinking about a parasitic organism residing within the cells of their brain. Yet, roughly 15–30% of the U.S population and up to a staggering 80% of the populations in France and Brazil are infected with the protozoan parasite Toxoplasma gondii.
This persistent little pathogen typically goes undetected in normal healthy adults because the immune system keeps the infection from ever getting out of control. However, T. gondii is particularly dangerous to immunosuppressed individuals and during pregnancy. Infection in pregnant women can cause severe congenital defects and even death of the fetus. Chronic infection with T. gondii parasites has two main components—the unicellular parasite and the tissue inflammation it causes.
Now, a team of researchers at the University of California, Riverside reports on their new findings that Toxoplasma infection leads to a disruption of neurotransmitters in the brain, as well as postulating a trigger that leads to neurological disease in those already predisposed to such a disease.
The UC Riverside team found that Toxoplasma infection leads to a significant increase in glutamate, the primary and most important neurotransmitter in the brain, which transmits excitatory signals between neurons. This glutamate increase is extracellular and is strictly controlled by specialized cells in the central nervous system called astrocytes. Interestingly, glutamate buildup is seen in traumatic brain injury as well as highly pathological and neurodegenerating diseases such as epilepsy, multiple sclerosis, and amyotrophic lateral sclerosis (ALS).
One role astrocytes play is to remove extracellular glutamate, lest it increase to pathological levels that could damage neurons. This is primarily achieved using a glutamate transporter, called GLT-1, tasked with regulating extracellular glutamate. GLT-1 soaks up glutamate released by neurons and converts it back into the safer substance glutamine, which can then be used by cells for energy.
“When a neuron fires it releases glutamate into the space between itself and a nearby neuron,” explained senior study author Emma Wilson, Ph.D., associate professor in the Division of Biomedical Sciences at UC Riverside School of Medicine. “The nearby neuron detects this glutamate which triggers a firing of the neuron. If the glutamate isn't cleared by GLT-1, then the neurons can't fire properly the next time, and they start to die.”
The investigators found that astrocytes swell during Toxoplasma infection and are not able to regulate extracellular glutamate concentrations. Furthermore, GLT-1 is not expressed correctly. This leads to a buildup of the glutamate released from neurons and the neurons misfire.
“These results suggest that in contrast to assuming chronic Toxoplasma infection as quiescent and benign, we should be aware of the potential risk to normal neurological pathways and changes in brain chemistry,” Dr. Wilson noted.
The findings from this study were published recently in PLoS Pathogens in an article entitled “GLT-1-Dependent Disruption of CNS Glutamate Homeostasis and Neuronal Function by the Protozoan Parasite Toxoplasma gondii.”
Surprisingly, when the researchers treated the infected mice with ceftriaxone, an antibiotic known to produce beneficial results in mouse models of ALS, as well as neuroprotection in a variety of central nervous system injuries, they found that GLT-1 was upregulated. Restoring GLT-1 expression significantly reduced extracellular glutamate from pathological to standard concentrations, returning neuronal function to a normal state.
“We have shown for the first time the direct disruption of a major neurotransmitter in the brain resulting from this infection,” remarked Dr. Wilson. “More direct and mechanistic research needs to be performed to understand the realities of this very common pathogen.”
The next step for the UC Riverside team will be to dive into what initiates the downregulation of GLT-1 during chronic Toxoplasma infection.
“Despite the importance of this transporter to maintaining glutamate homeostasis, there is little understanding of the mechanism that governs its expression,” Dr. Wilson stated. “We'd like to know how cells, including peripheral immune cells, control the parasite in the brain. Toxoplasma infection results in the lifelong presence of parasitic cysts within the neurons in the brain. We'd like to further develop a project focused on killing the cysts, which is where the parasite hides from the immune response for the rest of the infected person's life. Getting rid of the cyst removes the threat of reactivation of the parasite and the risk of encephalitis while also allowing us to minimize chronic inflammation in the brain.”
Mysteriously, the parasite that causes toxoplasmosis can reproduce sexually only in cats. Asexually, it can replicate and live in any mammalian cell that has a nucleus. Indeed, the parasite has been found in every mammal ever tested.
While researchers have been noticing more recently that T. gondii is not nearly as latent or dormant as once presumed, Dr. Wilson noted that infection is no cause for major worry stating that “we have been living with this parasite for a long time. It does not want to kill its host and lose its home. The best way to prevent infection is to cook your meat and wash your hands and vegetables. And if you are pregnant, don't change the cat litter.”