![Model illustrates clinical implications of BCBM CTC screening method for brain micrometastases before they become detectable by MRI. BCBM-associated CTCs can be used as a tool to evaluate responses to therapy for BCBM patients. [Houston Methodist]](https://genengnews.com/wp-content/uploads/2018/08/Aug4_2017_HoustonMethodist_BCBMCTCScreeningMethod2212271167-1.jpg)
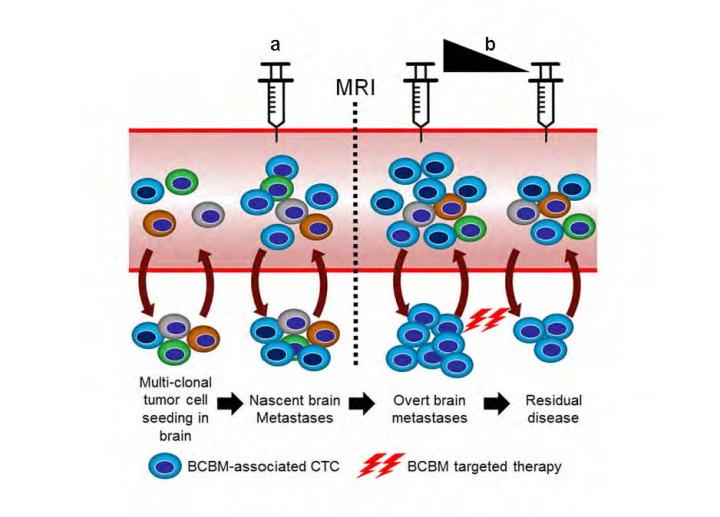
Model illustrates clinical implications of BCBM CTC screening method for brain micrometastases before they become detectable by MRI. BCBM-associated CTCs can be used as a tool to evaluate responses to therapy for BCBM patients. [Houston Methodist]
Scientists at the Houston Methodist Research Institute say their identification of circulating tumor cells (CTCs) in the bloodstream of patients who have breast cancer brain metastases could lead to the creation of more sensitive screening tools. More specifically, they hope to develop a blood test that can identify breast cancer patients at increased risk for developing brain metastasis and that can follow disease progression and response to treatment in real time.
They reported their study (“Molecular Characterization of Breast Cancer CTCs Associated with Brain Metastasis”) in Nature Communications.
“,,,we discovered a unique ‘circulating tumor cell gene signature’ that is distinct from primary breast cancer tissues. Further dissection of the circulating tumor cell gene signature identified signaling pathways associated with BCBM [breast cancer brain metastasis] CTCs that may have roles in potentiating BCBM,” write the investigators. “This study proposes CTC biomarkers and signaling pathways implicated in BCBM that may be used either as a screening tool for brain micro-metastasis detection or for making rational treatment decisions and monitoring therapeutic response in patients with BCBM.”
“Our research confirmed that CTCs in breast cancer brain metastases are distinct from other circulating tumor cells. Moreover, unlocking the mystery of how these seeds of metastatic disease survive and thrive over a period of years, sometimes decades, is an enigma in cancer,” said Dario Marchetti, Ph.D., senior author and director of the biomarker research program at the Institute. “Now we can take this information and develop a more sensitive screening tool to detect metastatic cancer in the blood, possibly even before metastasis is radiologically detectable by MRI [magnetic resonance imaging].”
“Our lab is the first in this field to perform a comprehensive report of patient-derived circulating tumor cells at the gene expression level, so we now have a clearer picture of the signaling pathways that allows them to establish brain metastases,” added Debasish Boral, Ph.D., the paper's first author and a research associate with the biomarker research program at Houston Methodist Research Institute.
“By comparing the whole-genome expression patterns of CTCs isolated from patient blood samples diagnosed with or without BCBM, we uncovered a 126-gene signature that is specific to these brain metastatic CTCs.”
The team now plans to increase the study patient population while looking to develop two types of liquid biopsies. One could be used by doctors as a screening technique to predict brain metastasis before the disease is detectable by MRI and the other to monitor treatment efficacy in patients diagnosed with brain metastasis.