![Mesenchymal stem cells have been labeled with ferumoxytol using a biomimicry method. The new method spares cells the rigors of transfection agents and electroporation, and it can be used to evaluate stem cell therapies better in preclinical and clinical trials. [Carnegie Mellon University]](https://genengnews.com/wp-content/uploads/2018/08/May19_2016_CarnegieMellonUniversity_MesenchymalStemCells1221865922-1.jpg)
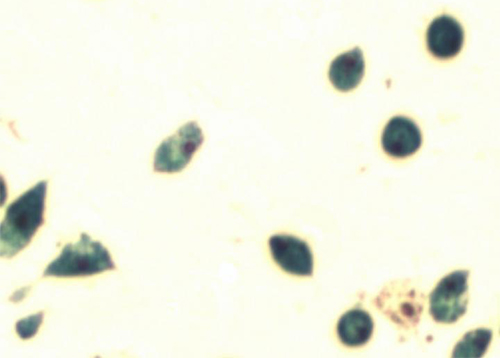
Mesenchymal stem cells have been labeled with ferumoxytol using a biomimicry method. The new method spares cells the rigors of transfection agents and electroporation, and it can be used to evaluate stem cell therapies better in preclinical and clinical trials. [Carnegie Mellon University]
If they are to be evaluated properly, stem cells that are deployed clinically need to be labeled. Even better, stem cells need to internalize tracking labels that can be picked up by means of magnetic resonance imaging (MRI). Yet stem cells such as mesenchymal stem cells (MSCs) seem to object to force-feeding, at least in culture. In their native environments, in vivo, these stem cells retain their appetites, their engulfing behaviors.
Suppose, reasoned scientists based at Carnegie Mellon University (CMU), MSCs in culture could be made to feel so much at home that they would happily scarf down an iron oxide nanoparticle. It might be possible to create stem cells for clinical use without resorting to force-feeding—via transfection agents or electroporation—which tends to produce stem cells of different sizes and functionalities. Most important, setting the table appropriately for stem cells would encourage them to take in labels that would allow researchers to assess how well they migrate through and become integrated with host tissues.
Led by Chien Ho, Ph.D., professor of biological sciences, the CMU scientists created an environment in a petri dish that resembled the environment inside the body. Dr. Ho’s team began by using traditional methods to extract cells from bone marrow, separate the MSCs from the other cells, and expand the number of MSCs. His team then devised a new way to culture MSCs by introducing other cells from the bone marrow,
The CMU scientists presented their results May 18 in the journal Scientific Reports, in an article entitled, “A New Method for Preparing Mesenchymal Stem Cells and Labeling with Ferumoxytol for Cell Tracking by MRI.”
“Here, we are reporting a new ‘bio-mimicry’ method by making use of the ‘in-vivo environment’ of MSCs to prepare native MSCs, so that (i) the phagocytic activity of cultured MSCs can be recovered and expanded MSCs can be ex-vivo labeled with Ferumoxytol, which is currently the only FDA approved SPIO [superparamagnetic iron oxide nanoparticles] nanoparticles for human use,” wrote the article’s authors. “Using our new method, 7-day cultured MSCs regain the capability to take up Ferumoxytol and exhibit an intracellular iron concentration comparable to that obtained by using Ferumoxytol–heparin–protamine nanocomplex; and (ii) cells can be re-sized to more native size.”
MSCs can be used to generate bone, cartilage, and fat cells and have promise for repairing bone and cartilage, damaged heart cells, and treating inflammatory and autoimmune diseases. More than 360 registered clinical trials are using MSCs, but the results have been mixed, with some patients reacting well and others not responding to the stem cell treatment. To understand why these results can be so variable, researchers need to be able to track the stem cells as they migrate through the body to see if they reach and graft to the appropriate site.
To date, researchers have not been able to label MSCs with ferumoxytol in cell culture (ex vivo) without the help of a transfection agent. Transfection agents are undesirable because they can change the cells' biology and inhibit their effectiveness. Furthermore, researchers have had difficulty culturing the large amount of cells needed for clinical dosing. Current methods also result in cells of different sizes and functionalities. Smaller, round cells are preferable because they show a higher capacity for regeneration and differentiation.
The alternative technique developed by Ho’s team, however, allows MSCs to retain their optimal size and regeneration capabilities and can internalize ferumoxytol for cell tracking. “Our method, the CMU scientists concluded, “can be very useful for expanding MSCs and labeling with Ferumoxytol, without the need for transfection agents and/or electroporation, allowing cell-tracking by MRI in both pre-clinical and clinical studies.”