Although the cell’s signaling networks may seem extravagantly complicated, they can be economical, too. For example, a protein known to comb nuclear DNA for defects has been found to latch onto cytoplasmic DNA—triggering a repair mechanism in one circumstance (preserving the cell's DNA) and an antiviral response in the other (attacking foreign DNA). This protein, called Rad50, serves double duty. Nature, it seems, saw no need to invent two DNA sensors when one would do for two very different signaling pathways.
This curious finding emerged from research accomplished at the Technische Universität München (TUM) and Ludwig-Maximilians-Universität München (LMU). According to TUM and LMU scientists, Rad50 in the cytoplasm serves as a kind of alarm mechanism, alerting the innate immune system to the presence of foreign DNA. Ordinarily, the cytoplasm is free of DNA. If any should be present, it is likely from a virus.
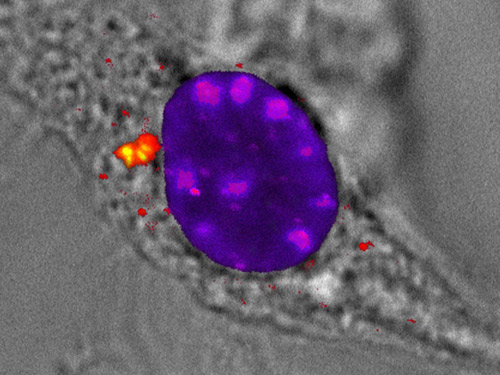
In their experiments, the participating scientists infected immune cells with a virus that introduced its DNA into the cytoplasm. They were able to show that Rad50 bound to the viral DNA in the cytoplasm, even though it normally docks onto damaged DNA in the cell nucleus. A crucial factor was that Rad50 interacted with a specific signal protein (CARD9) of the immune system at the same time, forming a complex.
“It is very surprising even for us that Rad50, which specializes in DNA in the cell nucleus, also detects foreign viral DNA and acts as a connecting link for the corresponding immune response,” said Jürgen Ruland, Ph.D., study leader and professor of clinical chemistry at TUM. Following up on this result, the researchers went on to define a cytosolic DNA-recognition pathway for inflammation and a physical and functional connection between a conserved DNA-damage sensor and the innate immune response to pathogens.
The researchers presented their work April 28 in Nature Immunology, in an article entitled “Rad50-CARD9 interactions link cytosolic DNA sensing to IL-1β production.” The article describes how the Rad50-CARD9 complex that they had discovered led to activation of a signal transduction pathway that ended with production of the messenger substance interleukin 1β (IL-1β).
“Transfection of dendritic cells with dsDNA or infection of dendritic cells with a DNA virus induced the formation of dsDNA-Rad50-CARD9 signaling complexes for activation of the transcription factor NF-κB and the generation of pro-IL-1β,” wrote the study’s authors. IL-1β, a vital “global player” of the immune system, is responsible for the onset of fever as a defense mechanism against pathogens, but also has a role in autoimmune diseases, such as rheumatoid arthritis.
In order to confirm their results, the researchers then used cells containing either no Rad50 or no CARD9, and again introduced DNA into their cytoplasm. Both cell types then produced far less interleukin 1β, as the Rad50-CARD9 complex could not be formed in order to activate the alarm system.
“Too much or too little of IL-1β can lead to a defective immune response or chronic disease, so its production must be strictly regulated by the body,” explained Dr. Ruland. “Now that we know Rad50 and CARD9 are important triggers for the alarm system and IL-1β production, we can gain a better understanding of many immune responses and develop strategies to influence them therapeutically.”