More than half a century ago, promising research on psychedelic drugs ran afoul of legislation declaring that such drugs had “no currently accepted medical use.” Although the legislation was meant to curb the illicit use of psychedelic drugs by members of the general population, it had an unfortunate side effect: It discouraged laboratory tests and clinical trials. Today, however, psychedelic drugs are making a comeback.
New research indicates that psychotropic substances can improve mental well-being by enhancing neuroplasticity, that is, the brain’s ability to make new neuronal connections. Proponents cite emerging data about the speed with which psychedelic medications can achieve lasting benefits, even among patients suffering treatment-resistant disorders such as depression. At the same time, there are those who warn of potentially harmful effects such as hallucinations and organ toxicities. However, many agree that psychedelic medications present mind-blowing opportunities.
These opportunities are being explored by the experts quoted in this article. Some of these experts are rationally designing modified psychedelic compounds to reduce off-target toxicities. Some are developing non-hallucinogenic versions that could be orally bioavailable as take-home medicines. And some are demonstrating the advantages of combining psychedelic medications with psychological therapy. From a business standpoint, strategizing to form partnerships could help accelerate and partially de-risk development of psychedelic medicines.
Targeting hallucinogenic receptors
Determining whether psychedelics could be the next therapeutic game changer will depend on the balance of benefits and risks. “I think the main promise with psychedelics is their unique activity in the brain,” says Jacqueline von Salm, PhD, co-founder and CSO, Psilera. “Initial research has shown that they can increase neuronal connections and even create new ones. This has the potential to help humans process memories and emotions in a healthier way, possibly leading to better mental health and addiction treatments.
“This unique activity could also help us find better cures for neurodegenerative diseases like dementia and Alzheimer’s disease. We have never had a major breakthrough in neurologically focused brain medicines. I think psychedelics could change that.”
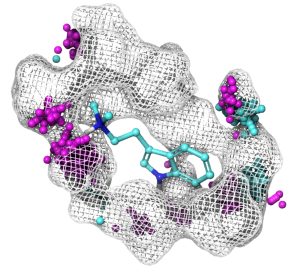
analogues interacting with key amino acids within the serotonin 2A receptor binding pocket.
According to von Salm, psychedelic therapeutics could be deployed more widely if certain research challenges were addressed. “Our company is focused on researching whether hallucinations are necessary for the therapeutic benefits of psychedelics,” she relates. “Hallucinations are a major side effect along with cardiotoxicity, stomach irritations, and/or effects on circadian rhythm (sleep).”
Psilera scientists are also studying how psychedelics actually work at different receptors in the brain and throughout the body. Although the precise mechanism of action for hallucinogens remains unclear, the receptor for serotonin (5-hydroxytryptamine [5-HT]) seems to be key for many of them. Serotonergic hallucinogens such as psilocybin (the primary active compound in “magic mushrooms”), lysergic acid diethylamide (LSD), and N,N-dimethyltryptamine (DMT) specifically target the 5-HT2A serotonin receptor.
Currently, Psilera scientists are designing compounds with reduced hallucinogenic effects at therapeutic dosages. “There has not been a lot of research of sub-hallucinogenic dosing of tryptamines and similar psychedelics,” von Salm notes. “We are focused primarily on understanding how these compounds interact with the 5-HT2A receptor and how that leads to positive behavioral outcomes.
“We are also interested in multiple other serotonin receptors specifically targeting learning and memory, as well as sigma receptors. Compounds like DMT and other tryptamine psychedelics have unique polypharmacology, and our hypothesis is that fine tuning which receptors are being hit, kind of like musical notes, could lead to interesting biological outcomes rather than a single-target approach.”
The company has synthesized over a dozen various tryptamines for testing in receptor assays and is choosing which compounds should be advanced to target mental health issues such as addictions, mood disorders, and neurodegenerative diseases.
Non-hallucinogenic psychoplastogens
Neuroscientists once thought that brain patterns were largely locked in after childhood. However, contemporary science reveals that new experiences can rewire the adult brain. Such neuroplasticity can both help and hurt. For example, bad experiences can drive deep depression, post-traumatic stress disorder, and many other mental pathologies.
Psychedelic medicines could selectively rewire pathological neural circuits. This possibility is being pursued by David E. Olson, PhD, chief innovation officer, Delix Therapeutics, and associate professor of biochemistry and molecular medicine at the University of California, Davis. “Unlike traditional approaches that haven’t changed for decades—such as SSRIs (selective serotonin reuptake inhibitors)—psychedelics and other psychoplastogens seem to produce rapid and sustained therapeutic effects after only one or a few doses,” he says. “Moreover, they are demonstrating efficacy in treatment-resistant populations, which is hugely important given that about one-third of all patients will not respond to traditional antidepressants.”
However, Olson points out that researchers still have a number of concerns. “The biggest issues,” he continues, “are related to scalability, equitable access, and safety.” He adds that in addition to addressing co-morbidities that can complicate treatment, researchers need to establish “appropriate protocols to mitigate the psychological, cardiovascular, and other risks associated with first-generation hallucinogenic compounds.”
Delix is addressing these challenges in several ways. Olson reports, “Delix is developing non-hallucinogenic variants as orally bioavailable take-home medicines that still produce rapid and sustained therapeutic effects. To identify these compounds, we use a combination of medicinal chemistry coupled with state-of-the-art assays relevant to neuroplasticity and hallucinogenic potential. By using first-generation hallucinogenic compounds as comparators, we can be confident that our compounds have similar therapeutic properties but without producing the subjective effects that have limited the scalability of compounds like ketamine and psilocybin.”
At present, the company is focusing on using its circuit-specific psychoplastogens to treat neuropsychiatric disorders, but it has a long-term vision of also tackling neurodegenerative disorders. Olson reveals, “Currently, we have two assets completing IND-enabling studies and plan to be in the clinic in 2023.”
Olson is optimistic about the future. “Psychedelic medicine has really reinforced the idea that we don’t have to be content with simply treating the symptoms of neuropsychiatric diseases,” he says. “We can move toward a truly healing-based approach, where one or a few doses of a compound can produce lasting beneficial effects.”
Rational drug design

Mindset Pharma
To develop improved therapeutic psychedelic compounds, Mindset Pharma is applying a methodological approach. “We are an early-stage drug discovery company that was formed to address what we saw as an unprecedented opportunity to develop new, optimized drugs in a field that had been largely off limits to a generation of researchers,” explains James Lanthier, CEO.
Inspired by known psychedelic structures, Mindset’s scientists have built a pipeline that focuses on four families of novel drugs for patients suffering from mood and psychiatric disorders. These include psilocybin-like conjugates as well as compounds similar to DMT and 5-methoxy-N,N-dimethyltryptamine 5-MeO-DMT). The latter two are hallucinogenic tryptamine drugs with effects similar to those of LSD.
Besides optimizing compounds, Mindset is considering the merits of different administration approaches. Lanthier says that some Mindset families include compounds that could advance psychedelic-assisted psychotherapy via a macrodosing approach. (With such an approach, the drug is taken under supervision in a specialized clinic. One drug that is already administered via macrodosing is psilocybin.) Lanthier adds that other Mindset families include sub-hallucinogenic compounds that could be taken at home on a regular basis, as are most psychiatric medicines at present. That is, the compounds could be administered via a microdosing approach.
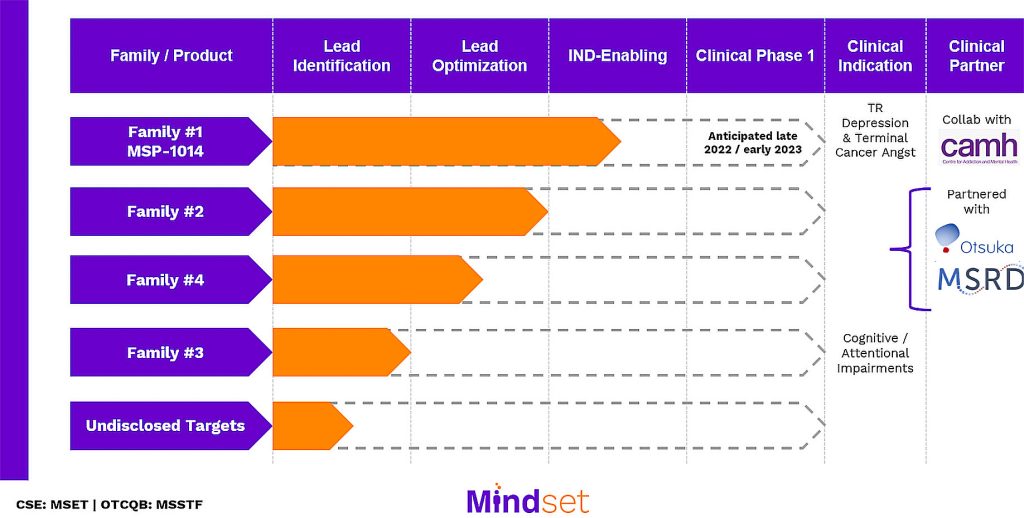
Garnering success in this arena will require strategic partnerships, Lanthier believes. “Next-generation drugs will need to pass through the standard regulatory process to be approved for therapeutic use, and as such, require investment and expertise,” he continues. “Mindset’s partnership with the McQuade Center for Strategic Research and Development (MSRD), a member of Otsuka Pharmaceuticals, is an example of the type of partnerships that can accelerate and partially de-risk the development of novel drugs.”
Although some industry observers say that the field of medical psychedelics is experiencing a renaissance, Lanthier emphasizes that “additional work needs to be done to better understand how these drugs will be used therapeutically.” He points out that significant research will have to be done to optimize the length and disposition of psychedelic interventions. “We envision that the future of psychedelic medicine may be highly personalized,” he declares. “That is why Mindset has focused on advancing multiple differentiated ‘families’ of new drugs that vary in duration and intensity.”
Compassionate and affordable help
At Compass Pathways, the need to overcome the challenges of accessing evidence-based and effective mental healthcare is emphasized by Ekaterina Malievskaia, MD, the company’s co-founder and chief innovation officer. She explains, “We started Compass Pathways to accelerate access to innovation for people living with mental health conditions who are not helped by existing therapies. We’re all about evidence, so our focus is on generating high-quality data needed to ensure new effective treatments are approved and broadly accessible within healthcare systems.”

Compass Pathways
The company’s first major initiative focuses on psilocybin therapy and has been designated a breakthrough therapy by the FDA. “Our lead indication is treatment-resistant depression (TRD),” Malievskaia elaborates. “We recently completed an international randomized controlled Phase IIb trial of COMP360 (our proprietary formulation of psilocybin, administered with psychological support) in 233 patients with TRD, and we presented data at the annual meeting of the American Psychiatric Association in May 2022.
“The results showed that a single 25 mg dose of COMP360 psilocybin, in combination with psychological support, was associated with a highly statistically significant reduction in depressive symptoms after three weeks (p < .001), with a rapid and durable response for up to 12 weeks. We are now getting ready to start Phase III pivotal trials that would hopefully lead to regulatory approval. We are also conducting Phase II studies in other areas of unmet need, specifically post-traumatic stress disorder and anorexia nervosa.”
Malievskaia notes that the company is working closely not only with regulators, but also with payers and healthcare systems to ensure a successful launch, should COMP360 psilocybin therapy be approved for use in the future. “But the task is bigger than simply getting psychedelics approved and broadly available,” she adds. “We aim to advance research in mental health to develop predictive, preventative, and precision models of care, accessible to all regardless of their ability to pay.”
Precision engineering
The therapeutic efficacy of psychedelic compounds can depend on the experiences they induce in patients. To ensure that these experiences are favorable, Mindstate Design Labs focuses on psychedelic compounds that can provide discrete and predictable states of mind.

Mindstate Design Labs
The company develops drugs that are meant to be delivered in a supervised therapy setting, the better to produce acute changes to mood and cognition. “It is the quality of the acute experience that drives treatment outcomes,” says Dillan DiNardo, the company’s CEO. “Our focus is the design of the altered state of consciousness which shapes that experience.”
DiNardo recognizes that the primary challenge in the development of novel psychedelic-assisted therapies is the lack of a useful translational model that predicts effects in humans.
“While the head-twitch response in rodents might show 5-HT2A activity, the effects of different psychedelic compounds in humans vary widely,” he notes. “No animal model can provide a useful indication of, for example, which variety of oceanic boundlessness (‘ego loss’) a new compound or combination will produce in humans.”
To meet this challenge, the company developed Osmanthus, a predictive modeling platform for the identification of drug targets and the precision design of modified conscious states. DiNardo reports, “Osmanthus is powered by human experience, using a combination of natural history, natural language processing, and biochemical data to map the biological basis of the diversity of psychedelic effects. We then match the psychedelic effect to the indication that is most suited to its application.”
Mindstate’s lead program consists of a combination of compounds designed to produce the entactogenic (“ecstasy”) effect of MDMA (3,4-methylenedioxymethamphetamine) with a superior side-effect profile. To advance the program, the company is conducting investigational new drug–enabling studies. It expects Phase I trials to start in 2023.
“The lead indication is treatment-resistant post-traumatic stress disorder,” DiNardo relates. “Following a second Phase I combination study, we plan to quickly expand to a number of additional programs targeting prevalent indications such as depression as well as various orphan indications in mental and behavioral health.”
Intranasal ketamine
Many are familiar with ketamine as an FDA-approved anesthetic. However, subanesthetic doses are being employed for treatment of depression, pain, and substance abuse disorders. Seelos Therapeutics is developing SLS-002, an intranasal racemic ketamine. Racemic refers to a mixture containing equal amounts of left- and right-handed enantiomers of a chiral molecule.
SLS-002 promises to treat acute suicidal ideation and behavior (ASIB). If the drug succeeds, it could help many people, suggests Raj Mehra, PhD, chairman and CEO at Seelos. He points out that the Agency for Healthcare Research and Quality has established that there were more than 1,000,000 visits to emergency rooms for suicide attempts in 2019 in the United States alone.
“The greatest challenge patients face is having a rapid acting antidepressant and anti-suicidality drug,” Mehra stresses. “Currently, all antidepressants are slow acting, take weeks to show efficacy, and are not anti-suicidal. SLS-002 is looking to address both of these challenges through its rapid action within 24 hours.”
According to Mehra, Seelos is pursuing two investigational new drug applications for the treatment of ASIB in major depressive disorder or post-traumatic stress disorder. He reports, “Experimental studies suggest ketamine has the potential to be a rapid, effective treatment for depression and suicidality.”
In contrast to serotonergic compounds, ketamine acts on the brain’s glutamate system and NMDA (N-methyl-d-aspartate) receptors involved in memory and learning. Some consider it a nonclassical psychedelic that helps “reset” the brain in a helpful way.
“Collectively, we need to raise the level of awareness of the therapeutic value of psychedelic medicine with all stakeholders, from patients, caregivers, physicians, nurses, psychologists, other health professionals, policy makers, to public health officials, and many others,” Mehra declares. “We need to destigmatize these conditions and invest in scientifically rigorous approaches to clinical development. To accomplish this, we must manifest a holistic approach that is truly patient centric—an approach that embraces and invests in the novel concepts that are emerging as legitimate treatments in psychedelic medicine.”

