![Left: activated B cells in mouse spleen. Right, top: synthetic immune organ that enables rapid proliferation and activation of B cells. Right, bottom: B cell viability and distribution 24 hours post-encapsulation. [Singh Lab]](https://genengnews.com/wp-content/uploads/2018/08/June11_2015_SinghLab_ExVivoImmuneOrganoids1284814671-1.jpg)
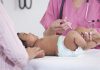
Left: activated B cells in mouse spleen. Right, top: synthetic immune organ that enables rapid proliferation and activation of B cells. Right, bottom: B cell viability and distribution 24 hours post-encapsulation. [Singh Lab]
Though an artificial device, a human-engineered immune organ is poised, its creators say, to descend on the immunotherapeutic stage, resolving longstanding questions about B cell maturation and hastening the translation of new classes of drugs. Were such a happy ending to be realized, few would mind that it depended on something so contrived as a hydrogel reinforced with silicate nanoparticles and seeded with cells.
A functional, synthetic immune organ that produces antibodies and can be controlled in the lab has been developed by Cornell University engineers. The organ, which mimics the anatomical microenvironment of lymphoid tissue and operates completely separate from a living organism, debuted June 3 in the journal Biomaterials, in an article entitled, “Ex vivo Engineered Immune Organoids for Controlled Germinal Center Reactions.”
The article describes synthetic organoids that are bio-inspired by secondary immune organs such as lymph node or spleen. Like real immune organs, these organoids convert B cells—which make antibodies that respond to infectious invaders—into germinal centers, which are clusters of B cells that activate, mature, and mutate their antibody genes when the body is under attack.
“Here we describe a B cell follicle organoid … that provides the basis to induce an accelerated germinal center (GC) reaction by continuously providing extracellular matrix (ECM) and cell-cell signals to naïve B cells,” wrote the authors of the Biomaterials article. “Compared to existing co-cultures, immune organoids provide a control over primary B cell proliferation with ∼100-fold higher and rapid differentiation to the GC phenotype with robust antibody class switching.”
The Cornell team, led by Ankur Singh, Ph.D., assistant professor of mechanical and aerospace engineering, emphasized that it was able to control the germinal process in the artificial organoids and tune how quickly B cells proliferated, became activated, and changed their antibody types.
Artificial immune organs could led to increased understanding of B cell functions, an area of study that typically relies on animal models to reveal how the cells develop and mature. What’s more, Dr. Singh asserted, such organs could be used to study specific infections and how the body produces antibodies to fight those infections—from Ebola to HIV.
“You can use our system to force the production of immunotherapeutics at much faster rates,” Dr. Sing stated. Such a system also could be used to test toxic chemicals and environmental factors that contribute to infections or organ malfunctions.
The process of B cells becoming germinal centers is not well understood, and in fact, when the body makes mistakes in the genetic rearrangement related to this process, blood cancer can result.
“In the long run, we anticipate that the ability to drive immune reaction ex vivo at controllable rates grants us the ability to reproduce immunological events with tunable parameters for better mechanistic understanding of B cell development and generation of B cell tumors, as well as screening and translation of new classes of drugs,” Dr. Singh explained.