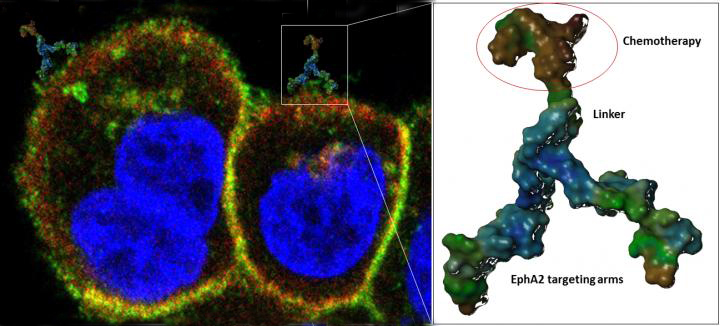
Cancer presents a moving target called metastasis that keeps ducking countermeasures. But metastasis can be targeted, animal studies have shown, by agents that bind to the surface proteins that are found on circulating cancer cells. According to a new study, one such agent, called 123B9, can be linked to a chemotherapeutic drug, paclitaxel, resulting a new and potentially effective countermeasure against metastatic cancer.
Cancer drugs usually target stationary targets such as tumors. But when cancer drugs are is conjugated with 123B9, an agent developed by researchers at the University of California, Riverside (UCR), they may be conveyed to circulating cancer cells. A UCR team led by Maurizio Pellecchia, Ph.D., a professor of biomedical sciences, had already demonstrated as much. Yet the team’s 123B-drug conjugates lacked sufficient killing power.
Then then the team conjugated 123B9 with paclitaxel to create an anticancer weapon that has more promise. This work appeared February 22 in the Journal of Medicinal Chemistry, in an article entitled “A Potent EphA2 Agonistic Peptide-Drug Conjugate Reduces Circulating Cancer Cells and Metastases in Breast Cancer Models.”
“While our studies indicated that YSA- or 123B9-drug conjugates can selectively deliver cytotoxic drugs to cancer cells in vivo, the relatively low cellular agonistic activity (high micromolar) of the agents for the EphA2 receptor remained a limiting factor to warrant further development of these PDCs [peptide–drug conjugates] in the clinic,” the article’s authors wrote. “Here we report that a dimeric version of 123B9 can induce receptor activation at nanomolar concentrations.”
Tumor metastasis is a leading cause of patient morbidity and mortality, and no treatments are currently available that specifically target metastasis formation. Cancer cells depend on a number of oncogenes, like EphA2, to form metastases, the medical term for cancer cells spreading from the primary site to other regions in the body, accomplished when these cells break away from the primary site, travel through the blood or lymph system, and form new tumors elsewhere in the body.
Dr. Pellecchia and his colleagues found that when 123B9 binds to the extracellular region of the EphA2 receptor expressed in cancer cells, it causes the oncogene to internalize and degrade inside the cell, thus preventing cancer cells from entering circulation and metastasizing. “Because this binding causes EphA2 internalization,” Dr. Pellecchia explained, “we also sought to conjugate 123B9 with paclitaxel and thus direct the drug to migrating cancer cells.”
Recent collaborative work between UCR and Cedars-Sinai Medical Center in Los Angeles demonstrated that in animal models of human breast cancer, mice treated with 123B9 that was conjugated with paclitaxel had significantly fewer circulating cancer cells in the blood compared to mice that were not treated or even treated with paclitaxel alone.
“Our work predicts that reducing the number of circulating cancer cells produces less metastasis,” Pellecchia asserted. “Indeed, in a second tumor model of metastatic breast cancer, we demonstrated that mice treated with the EphA2-targeting paclitaxel conjugate presented nearly no lung metastases, while a large numbers of lesions were observed in both untreated mice and in mice treated with just paclitaxel.”
“We demonstrated that conjugation of dimeric 123B9 with paclitaxel is very effective in targeting circulating tumor cells and inhibiting lung metastasis in breast cancer models,” the authors of the current study concluded. “These studies represent an important step towards the development of effective EphA2-targeting PDCs.”
Dr. Pellecchia cautioned that the road to a therapeutic for human trials is still long and includes the iterative design and synthesis of more potent and selective agents. “Nonetheless,” he continued, “the proof-of-concept studies we have obtained thus far are extremely encouraging, and we are confident that with proper support and efforts we could translate our findings into experimental therapeutics for a variety of solid tumors that are driven by EphA2 overexpression, including breast, lung, prostate, pancreatic, and ovarian cancers.”