![Immunofluoresence image of cytotoxic T cell (left) engaging a cancer cell (round cell, center). Labels: actin (green), lysosomes (red), nuclei (blue) [NIH]](https://genengnews.com/wp-content/uploads/2018/08/FARE_Ritter2132502191-1.jpg)
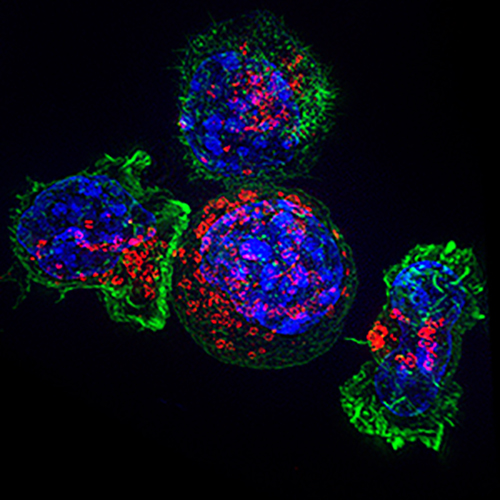
Immunofluoresence image of cytotoxic T cell (left) engaging a cancer cell (round cell, center). Labels: actin (green), lysosomes (red), nuclei (blue) [NIH]
The importance of cytotoxic T cells—colloquially known as killer T cells—in destroying cancer cells cannot be overstated. Our immune system employs an army of these specialist immune cells to protect the body from external threats, such as invading viruses and bacteria, as well as from internal threats, such as malignant tumor cells. Researchers are trying to harness these T cells as a way to fight cancer, programming them to recognize a patient's cancer cells rapidly. Scientists grow the T cells in the laboratory in large numbers and then reintroducing them into the body to destroy the tumor—an approach known as adoptive T-cell immunotherapy.
However, this approach has been hindered by the fact that killer T cells are short-lived—most killer T cells are gone within 3 days of the transfer. Now, a collaborative team of scientists led by investigators at the University of Cambridge has recently discovered a small molecule that can turn short-lived killer T cells into long-lived, renewable cells that can last in the body for extended periods of time—a scenario that could dramatically improve cell-based immunotherapy approaches.
“In a sense, this means that rather than creating killer T cells that are active from the start, but burn out very quickly, we are creating an army of 'renewable cells' that can stay quiet for a long time, but will go into action when necessary and fight tumor cells,” explained senior study investigator Randall Johnson, Ph.D., professor of molecular physiology and pathology at the University of Cambridge and a Wellcome Trust principal research fellow.
In the new study—the findings of which were published recently in Nature in an article entitled “S-2-Hydroxyglutarate Regulates CD8+ T-Lymphocyte Fate”—the researchers identified a new role for a molecule known as 2-hydroxyglutarate, or 2-HG, which is known to trigger abnormal growth in tumor cells.
Interestingly, the research team showed that a slightly different form of the molecule also plays a regular, but critical, role in T-cell function—it can influence T cells to reside in a memory state. This is a state where the cells can renew themselves, persist for a very extended period, and reactivate to combat infection or cancer.
“We show that CD8+ T-lymphocytes accumulate 2-hydroxyglutarate in response to T-cell receptor triggering,” the authors wrote. “This increases to millimolar levels in physiological oxygen conditions, via a hypoxia inducible factor 1 alpha-dependent mechanism. S-2-hydroxyglutarate predominates over R-2-hydroxyglutarate in activated T cells, and we demonstrate alterations in markers of CD8+ T-lymphocyte differentiation in response to this metabolite.”