The bacterium causing leprosy, Mycobacterium leprae, has been next to impossible to study because of extreme difficulties associated with its culturing and the lack of animal models. A particularly vexing question that remains unanswered is how M. leprae, an obligate intracellular pathogen, inflicts damage to separate tissues and organs around the body. The present study provides a twofold breakthrough in this field. The authors* were not only able to create a model for the infection using mouse Schwann nerve cells, but in the course of their studies the team also discovered a fairly unexpected mechanism by which the mysterious bacteria invade human tissues. Through incubation of isolated Schwann cells with M. leprae, the authors found that the bacteria trigger reprogramming of the adult nerve cells, turning them to a progenitor/stem-like type (Figure 1).
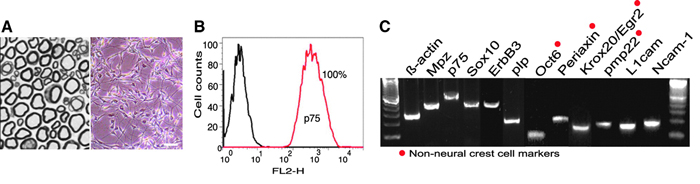
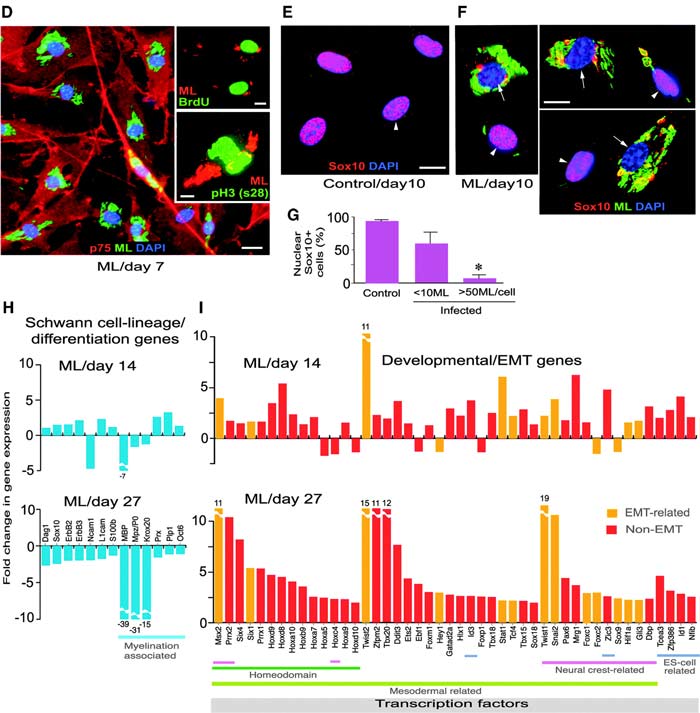
These cells, in turn, can detach from their typical structures comprising the sheaths of motor and sensory neurons and, given their plasticity and newly acquired mesoderm characteristics, migrate to distal sites and re-establish a site of infection and tissue damage through redifferentiation. This mechanism was verified by the authors through in vitro testing using co-culturing and in vivo testing using a nude mouse model (Figure 2).
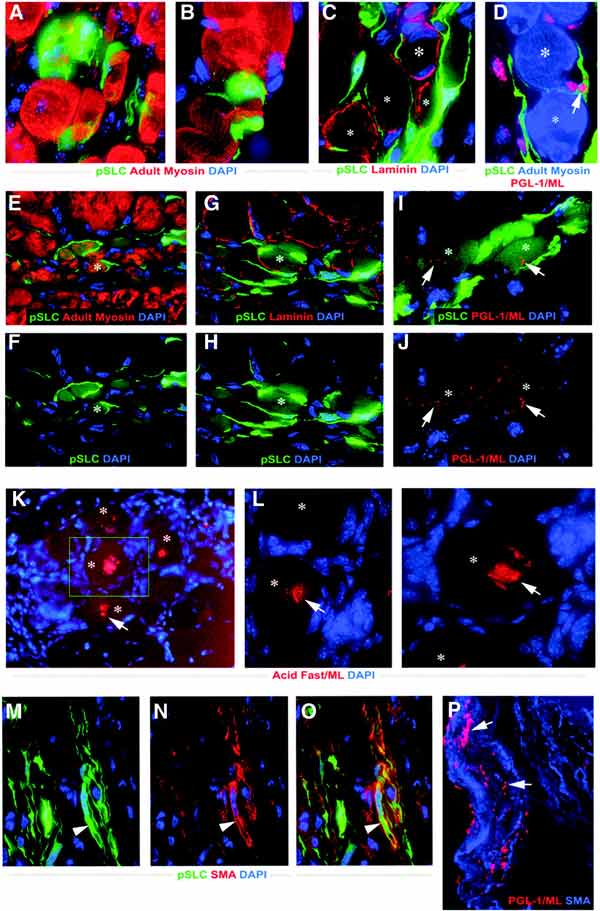
Figure 2. Redifferentiation of reprogrammed progenitor/stem-like cells (pSLC) contributes to passive bacterial transfer to skeletal muscles and smooth muscles in vivo. (A–D) Transverse frozen sections of tibialis anterior (TA) muscles injected with ML-infected GFP+ pSLC after 10 days. Deltavision images showed GFP + pSLC (green) either fused with myofibers (A, B) or migrating in between muscle fibers (C, D). Antibodies to adult myosin detected muscle fibers (red in A, B; blue in D) and laminin demarcated individual muscle fibers (red in C). Antibodies to PGL-1 detected ML (in red; arrow) associated closely with muscle fibers (D). Asterisks in all figures denote individual myofibers. (E–J; Deltavision images) Infected GFP+ pSLC were incorporated into regenerating muscles at 3 weeks post-injection. GFP + myofibers are positive for adult myosin (E, F) and are demarcated by laminin (G, H). pSLC incorporation passively transmitted ML to myofibers as detected by PGL-1+ ML (red; arrows) in GFP+ myofibers (I, J). (K, L) Bacterial presence within the skeletal muscle fibers (asterisks) was confirmed by acid fast mycobacterial staining (red). Arrows show clumps of rod-shaped ML in several individual muscle fibers. (M–P) Administered infected GFP+ pSLC differentiate into SMA+ smooth muscles in the dermal area. Antibody to SMA (red) colocalizes with differentiated GFP+ pSLC (green; arrowheads); merged image is shown in (O). (P) Higher magnification showed the PGL+ ML (red; arrows) within SMA+ smooth muscles (blue) near dermal vessels. Magnifications: (A–D, K, L) 60 × ; (E–J, M–O) 40 × ; (P) 100×.Although it still remains to be established how exactly the leprosy bacteria trigger the Schwann cell reprogramming, the new paradigm of bacterial colonization and spreading may have wide implications for our understanding of cell differentiation, tissue plasticity, and host–parasite interactions.
*Abstract from Cell 2013, Volume 152: 51–67
Differentiated cells possess a remarkable genomic plasticity that can be manipulated to reverse or change developmental commitments. Here, we show that the leprosy bacterium hijacks this property to reprogram adult Schwann cells, its preferred host niche, to a stage of progenitor/stem-like cells (pSLC) of mesenchymal trait by downregulating Schwann cell lineage/differentiation-associated genes and upregulating genes mostly of mesoderm development. Reprogramming accompanies epigenetic changes and renders infected cells highly plastic, migratory, and immunomodulatory. We provide evidence that acquisition of these properties by pSLC promotes bacterial spread by two distinct mechanisms: direct differentiation to mesenchymal tissues, including skeletal and smooth muscles, and formation of granuloma-like structures and subsequent release of bacteria-laden macrophages. These findings support a model of host cell reprogramming in which a bacterial pathogen uses the plasticity of its cellular niche for promoting dissemination of infection and provide an unexpected link between cellular reprogramming and host–pathogen interaction.
Anton Simeonov, Ph.D., works at the NIH.
ASSAY & Drug Development Technologies, published by Mary Ann Liebert, Inc., offers a unique combination of original research and reports on the techniques and tools being used in cutting-edge drug development. The journal includes a “Literature Search and Review” column that identifies published papers of note and discusses their importance. GEN presents here one article that was analyzed in the “Literature Search and Review” column, a paper published in Cell titled “Reprogramming adult Schwann cells to stem cell-like cells by leprosy bacilli promotes dissemination of infection”. Authors of the paper are Masaki T, Qu J, Cholewa-Waclaw J, Burr K, Raaum R, and Rambukkana A.





