October 1, 2011 (Vol. 31, No. 17)
John R. Birch, Ph.D.
Improvements in Microbial and Mammalian Systems Design Drive Advances in the Field
We now take it for granted that we can use recombinant DNA technology to express a wide range of proteins for use in many research and commercial applications, particularly in the field of human healthcare.
Before the recombinant revolution, there were a few proteins such as insulin and human growth hormone that could be manufactured by extraction from natural tissues, but many proteins of potential therapeutic interest could not be produced in sufficient quantity. A good example of this is interferon.1
Discovered in the 1950s, this family of proteins generated a huge amount of interest in the 1970s as potential antiviral and anticancer agents. There was a global effort to produce sufficient quantities in cell culture and from natural tissues but the quantities that could be made were small. In addition, it was a real challenge to produce enough material for clinical use.
Researchers at the Frederick Cancer Research Center, for example, reported that it required several thousand liters of cell culture to produce tens of milligrams of interferon. The picture changed dramatically in the 1980s when the genes for the different interferon species were cloned and expressed in microbial systems and the first recombinant interferon product made it to the market in 1986.

John R. Birch, Ph.D.
Plethora of Products
There are now over 200 biopharmaceuticals on the market in the U.S. and EU2 and many hundreds more in development. The first recombinant product, insulin3 (Eli Lilly), produced in E. coli, was approved in the U.S. in 1982. This was followed by other products expressed in that bacterium (human growth hormone-1985, interferon-a-1986) and in the yeast Saccharomyces cerevisiae (hepatitis B vaccine-1986).
While both of these organisms proved valuable and have been used extensively in the ensuing years, it became apparent quite early on that they would not be appropriate for the expression of all proteins. The first generation of products were typically small proteins, lacking post-translational modifications such as glycosylation that are commonly found on many mammalian proteins of therapeutic interest.
For large complex molecules, and particularly for proteins requiring mammalian-type glycosylation to be effective as therapeutics, microbial expression was not a viable option. For these proteins attention turned to mammalian cell culture and the first recombinant product (tissue plasminogen activator from Genentech) was approved in 1987.
As it turned out, mammalian cell culture would be used to produce a wide range of enzymes, blood factors, monoclonal antibodies and other proteins. In fact, cell culture is now used to produce more than half of the licensed proteins.
Monoclonal antibodies have had a particularly big impact on the development of mammalian cell expression technology. There was great interest in the therapeutic use of antibodies following the development of the monoclonal technology in the 1970s and a nonrecombinant murine antibody (OKT®3), produced in mouse hybridoma cells was licensed in 1986.
However, the more general use of antibodies was limited by their immunogenicity, a problem that was resolved using novel engineering approaches to produce chimeric, humanized, and eventually, fully human recombinant antibodies. There are now around 25 antibody therapeutics on the market, and as a class they represent approximately two-thirds of the biopharmaceutical proteins in development4.
In addition to numbers of products, antibodies have also had an impact in terms of quantities required. Because of the large doses needed for some products, manufacturing requirements can be high—tonnage quantities in a few cases. On the one hand this has led to a requirement for extremely large-scale culture systems (up to 20,000 liters in scale).5 On the other hand, it has been a potent driver for improving the efficiency of cell culture technology.
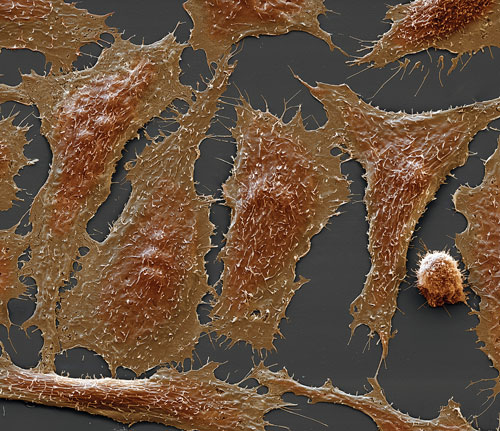
Scanning electron micrograph of chinese hamster ovary cells: The CHO cell line is one of the most commonly used in the biotechnological production of substances such as monoclonal antibodies. [Eye of Science/Photo Researchers]
CHO Cell Lines
The Chinese hamster ovary (CHO) cell line, first isolated in 1958 by Tjio and Puck, has become the most commonly used cell line for the production of recombinant proteins, including antibodies. A few other cell lines are also used, notably the mouse NS0 and Sp2/0 myeloma cell lines for production of antibodies.
A number of gene vector systems were developed for use in mammalian cell lines and among the best known are those based on the use of dihydrofolate reductase (DHFR) or glutamine synthetase (GS expression system™) as selectable markers.5 Within vectors are strong promoter elements that drive high expression. Vectors typically contain features that ensure that the product gene integrates into a transcriptionally efficient site in the cell’s genome, either by stringent selection or, in some cases, by directed integration.
It has also proved possible to use “insulating” sequences that ensure efficient expression regardless of integration site.
Efficient expression technology, coupled to smart screening of candidate cell lines (frequently based on automated high-throughput systems), permits the generation of stable cell lines with high-specific productivity.
Alongside these developments have been exceptional advances in fermentation technology, particularly in the area of culture medium design and feeding strategies for fed-batch culture. These advances in expression and process technology have led to improvements in productivity for antibodies of well over 100-fold in the last two decades. Titers of several grams per liter are now routinely achieved, with examples in excess of 10 grams per liter reported.6 Thirty years ago it was far from obvious that this could be achieved.
One of the biggest challenges with mammalian cell expression technology has been to develop highly productive cell lines in as short a time as possible. This is not a major issue for microbial systems. But in the early days of recombinant mammalian cell culture it could take one to two years to develop a stable cell line suitable for long-term production, and this had a serious impact on overall timelines.
Significant progress has been made by eliminating the need for rounds of gene amplification and reducing the time taken for establishing clonality and for screening. Nevertheless, it still takes several months to create a production strain and work continues to reduce timelines further. Rapid expression of proteins using transient transfection technology has been used for many years to produce small quantities of material for research.
Recent developments in the optimization of this technology have led to antibody titers in excess of 1 g/L as well as the suggestion that this may start a paradigm shift in the industrial production of proteins.7
Future Trends
Looking to the future, what trends are we likely to see? Given the high level of interest in antibodies and the number of monoclonals entering clinical trials, mammalian cell culture will remain a key technology for the foreseeable future.
We will also continue to see improvements to the technology both in terms of expression systems and culture processes. There is, for example, strong interest in improving the inherent properties of cells used for production. Examples include the CHOK1SV derivative of the CHO cell, adapted to grow in suspension in chemically defined medium.8
With increasing knowledge of those aspects of cell biology that influence the behavior of cells in a production process we are likely to observe an increasing use of cell-engineering approaches to improve the properties of cells.9 This includes properties that enhance the cell’s productive capabilities and others that improve product characteristics.
For example, an engineered variant of CHO has been created in which the gene for a-1, 6-fucosyl transferase (FUT8) has been knocked out.10 This variant is unable to add fucose to glycan structures on proteins and it turns out that this can improve the ADCC effector function of antibodies (a property that is potentially useful in a number of therapeutic applications).
While mammalian cell culture continues to be important, there is also an upturn in interest in microbial expression systems driven by product trends and progress in technology. On the product front there are, for example, new generations of engineered binding molecules based on antibody fragments and other protein scaffolds that are significantly smaller than antibodies and are produced in microbial culture.11, 12 Two antibody fragments, produced in E.coli, are already on the market: Cimzia® and Lucentis®.
Microbial expression technology has also progressed. A wider range of micro-organisms are now available, including engineered strains, that provide opportunities to select a host best suited to a given protein. For example, 2009 saw the first approval of a product (ecallantide) made in Pichia pastoris.2
A broader choice of expression technology also provides somewhat more flexibility in process design, e.g., whether the protein will be secreted or produced intracellularly.
There are significant advantages in the use of microbial systems: shorter process development timescales, less complex processes, and reduced risk of viral contamination. The drawbacks of microbial culture, which were observed 30 years ago, i.e., the difficulty of making large complex molecules like antibodies and the inability of microorganisms to provide human glycan structures on glycoproteins, remain challenging but are gradually being overcome. Whole antibodies have been expressed in E. coli13 and yeast, and Pichia pastoris has been glycoengineered to produce human glycan structures.14
In summary, the last 30 years have seen extraordinary progress in the field of recombinant expression. There is no reason to expect the next three decades to be any less exciting. Novel protein therapies and a continuing drive to improve process economics, shorten development timelines, and enhance product quality will ensure a continuing flow of advances in protein-expression technology.
References
1 Klein F, et al., Antimicrobial Agents and Chemotherapy, March 1979, p. 420-427
2 Walsh G, 2010, Nature Biotechnology 28: 917-924
3 Johnson, IS (1983) Science 219: 632-636
4 PhRMA survey 2008, Biotech Products Approved and in Development
5 Birch, JR and Racher, AJ (2006) Advanced Drug Delivery Reviews 58: 671-685
6 Huang, Y-M et al., (2010) Biotechnol Prog 26: 1400-1410
7 Backliwal, G et al., (2008) Nucleic Acids Research 36: e96
8 Rendall, M et al., (2005) in Godia, F and Fussenegger, M (eds) Animal Cell Technology Meets Genomics, Springer, Dordrecht, pp. 701-704
9 Lim, Y et al., (2010) Biotechnology and Applied Biochemistry 55: 175-189
10 Yamane-Ohnuki, N et al., (2004) Biotechnol Bioeng 87: 614-622
11 Enever, C et al., (2009) Current Opinion in Biotechnology 20: 405-411
12 Gill, DS and Damle, NK (2006) Current Opinion in Biotechnology 17: 653-658
13 Simmons, LC et al., (2002) J Immun Meth 263: 133-147
14 Gerngross, T (2004) Nature Biotechnology 22: 1409-1414
John R. Birch, Ph.D. ([email protected]), former CSO at Lonza Biopharmaceuticals, U.K., is an independent consultant based at Henley-on-Thames, U.K.







