September 1, 2012 (Vol. 32, No. 15)
Josh P. Roberts
The decision of how to put a transgene into a cell depends as much on the concerns about doing so as it does on the ease of doing so. Will the vector be able to find and enter its desired target? Will the transgene insert randomly into the genome, or become diluted out as the host cell replicates? Is the vector immunogenic? Can sufficient quantity of sufficient quality vector be produced?
What is perhaps transfection’s ultimate use—modifying the human organism—was front and center for researchers gathered at this year’s American Society for Gene and Cell Therapy annual meeting.
Effective analgesics have been in use for thousands of years, yet our ability to use them to treat localized pain is limited by interaction of the drug with other than the desired receptors. High doses of opiates, for example, will cause confusion, constipation, and urinary retention. Yet if the drugs could be delivered directly to the sites where they are needed, it may be possible to bypass such off-target effects.
David Fink, M.D., chair of the department of neurology at the University of Michigan, and his colleagues engineered NP2, a herpes simplex virus (HSV)-based vector, to express a naturally occurring opioid peptide. When injected into the skin the vector is picked up and transported by the sensory nerves to the dorsal root ganglia (DRG), where they take up residence in the nuclei as circular episomes. Enkephalin peptides—endogenous agonists for the delta opioid receptor—are produced, carried to axonal terminals, and released to the spinal cord.
“We chose herpes because, really, herpes is unique in being a virus that naturally targets DRGs,” explained Dr. Fink. Most people have HSV latent in their ganglia, and people live with recurrent cold sores (indicating the presence of wild type HSV in their sensory ganglia), for life. And the amount of nonreplicating recombinant vector that is being put into the skin—the natural site that the virus uses to infect—is orders of magnitude less than would be found in a cold sore. So “we don’t think it should cause problems, but that’s why we did a Phase I trial in patients with a terminal disease.”
Small molecule Phase I studies are traditionally done in normal peers, but gene therapy trials have to be carried out in a patient population. Because theirs was the first trial to use HSV to deliver a transgene, terminal cancer patients with intractable focal pain were chosen as the first recipients of NP2. There were no serious adverse events.
Patients receiving a high dosage of NP2 “had a very substantial reduction in their pain,” recounted Dr. Fink, with the average level dropping from almost 8 to less than 2 on a 10-point scale. “But there was no placebo control.” The results were encouraging enough for the company, Diamyd Medical, to sponsor a Phase II trial, which is currently under way with more patients and a placebo control.
In his most optimistic assessment, NP2 exemplifies for Dr. Fink a platform technology that could be used to deliver genes into sensory neurons to treat inflammatory pain, or neuropathic pain, or to prevent nerve damage; HSV-based vectors for these applications are currently being investigated.
The boundary of the approach, Dr. Fink says, is that it is only appropriate for problems that are focal in nature. It is “not a solution for somebody who has whole-body pain, like fibromyalgia.”
Industrial-Strength Gene Therapy
Industrialization of the gene therapy process—going from laboratory animals to clinical trials, and even more so making the leap from clinical trials to commercial product—is a challenge that most academic scientists rarely have to face. Rather than manipulating a few hundred thousand cells, “to treat a patient you need to manipulate 250 million cells,” points out Mitchell Finer, Ph.D., CSO at bluebird bio. “In every biological process there are issues surrounding scaling.”
Many early trails with lentiviral vectors—“including ours”—were done with a noninfective particle to infective particle ratio on the order of 2,000–5,000:1, which is “not a very highly potent drug,” said Dr. Finer. The company is now making vector under full GMP conditions with a particle to infective ratio about 10-fold less, allowing it to use about one-third the product “and still get three times the result that we saw previously.”
Bluebird claims to be the first company to migrate to stirred bioreactors for large-scale manufacture of pure, potent lentiviral vectors, producing the first such material to be used in the clinic, Dr. Finer says. “Many of the trials and tribulations of gene therapy have really been a failure to make a pharmaceutical-grade product. Now for lentivirus, we have such a product—we can make it at large enough scale so that we can treat 10, 20, 30 patients in a batch.”
The company reported efficacy and safety results of a β-thalassemia patient treated 54 months prior with a lentiviral vector encoding the human beta globin gene and control sequences enabling expression exclusively in the blood lineage. The patient has maintained hemoglobin levels, gene markings, and therapeutic benefit, and has been independent of the need for blood transfusions for four years. Another patient, treated in November, was reported to be on the same positive trajectory in terms of the presence of marked cells in her peripheral blood.
Vectors are being stored in anticipation of clinical trials for β-thalassemia to begin later this year or early next year in 20–25 patients in France and the U.S. A patient’s own bone marrow cells will be incubated with the vector at a centralized manufacturing facility. Most of the cells will be frozen in liquid N2 while rigorous quality control assays are performed. They will then be shipped to the hospital pharmacy and thawed at bedside to be re-infused into the patient.
Relieving Heartache
Rather than bring the target cells to the vector to treat recurrent angina pectoris, Gabor Rubanyi, M.D., Ph.D., CSO of Cardium Therapeutics, sends recombinant adenoviral vector to the heart. The concept is that the E1-deleted type 5 adenovirus containing recombinant human FGF-4 gene (driven by a CMV promoter) will deliver the gene, allowing growth factor protein to be produced where it is needed, he said. “This will stimulate or accelerate collateral vessel growth, so new vessels will be established in the heart.”
The concept has been tested in numerous Phase I, II, and III clinical trials over the course of 15 years, during which over 450 patients with coronary artery disease (angina) have had the Generx Ad5FGF-4 vector infused into their coronary arteries. “There were very good interim results in terms of efficacy for certain patient subgroups with myocardial ischemia, but overall the therapeutic efficacy was not overwhelming,” Dr. Rubanyi said.
“We observed that certain patients with more severe coronary artery disease responded better than patients with less severe disease. So we went from the bedside back to the bench to confirm these findings and to find a way to improve our Generx therapy.”
The trials showed a large interindividual variability—some things worked in some patients but not in others. While trying to parse out the reasons for this, they serendipitously discovered that a 75-minute coronary artery occlusion in pigs drastically increased vector uptake and transgene expression.
In a separate study using an occlusion/reperfusion model in pigs, a reporter-encoding adenoviral vector was injected into all the coronary arteries. Yet, Dr. Rubanyi explained: “most of the transfection occurred in the zone that was ischemic, which we occluded. The ischemic zone in pig heart mimics, in certain ways, the conditions present in patients with coronary artery disease.”
Building on that finding, the researchers set out to replicate the benefits of a prolonged occlusion in a way that could be used to benefit humans. They tried two short occlusions separated by a five-minute intermission (“even patients with angina will easily tolerate three minute total occlusion of the coronary artery”), and they tried vasodilation with nitro glycerin. Neither treatment by itself did the job, recalled Dr. Rubanyi, “but when we combined these two occlusions with nitro glycerin infusion, we saw the same increase in transfection efficiency as we have seen with long-term occlusion.”
Dr. Rubanyi puts forth several reasons why the protocol enhances Generx uptake. It will cause significant vasodilation, exposing more vessels and more surface area, and increased vessel permeability, allowing more virus to be taken up by the heart. “But more importantly,” he believes, is that the Coxsackie Adenovirus Receptor (CAR), normally buried in the tight junction, is exposed.
“When there is ischemia or any injury, then these tight junctions loosen up and these proteins all of a sudden are exposed and can bind the virus. Transfection starts with adenovirus fiber protein attaching to this receptor.”
Vector Agnosticism
Sangamo BioSciences, too, used an adenovirus for Phase I trials of its SB-728-T for HIV/AIDS therapy, but in a sense that doesn’t really matter. Because the genes that they deliver need only to be transiently transcribed to achieve their aim, “we have the luxury of using gene delivery approaches that are also transient in their nature,” said Philip Gregory, D.Phil., CSO and vp for research.
They use whatever makes sense for the application: for T cells a chimeric adenoviral vector designed to recognize T cells has worked best, they electroporate plasmid DNA or mRNA into bone marrow stem cells, and they use AAV vector to transfect the liver. “We can be quite agnostic in terms of vector, and quite inclusive because we don’t require a persistence in that tissue.”
The nonpersistence and nonintegration of vector means, among other things, that they need not worry about the random integration of vector (and all that entails in terms of transgene or endogenous gene silencing or endogenous gene activation). Nor is the immune response to vector or transgene an issue, as these wash out as the cells divide.
In the trials, T cells were treated ex vivo by delivering a transgene encoding both monomers of a zinc finger nuclease (ZFN) in a single cistron. The obligate heterodimeric protein—each monomer composed of a zinc finger DNA sequence-specific recognition domain and a nuclease domain taken from FOK1—recognizes and creates a double-stranded break in the CCR5 gene. The cell’s error-prone nonhomologous end joining (NHEJ) pathway then repairs the break, frequently creating a disruption during the process.
Researchers relied on the observation that the CCR5 protein seems to be virtually necessary for HIV entry into the host cell in that people who are homozygous mutant for CCR5 are naturally resistant to HIV infection. And, in what is seen as a proof-of-concept for gene therapy, an HIV patient with leukemia was “cured” of HIV after receiving a bone marrow transplant from a CCR5-mutant donor.
Dr. Gregory has no expectation of 100% protection from HIV—the majority of T cells will remain infectable. Only about 10% of the 10–30 billion T cells being returned to the patient will be CCR5-/-, yet those billion-plus T cells are possibly sufficient to protect the entire T-cell repertoire with a CCR5 bi-allelic modification, he said. “So we should potentially be able to protect every cell that recognizes any known epitope in the patient.”
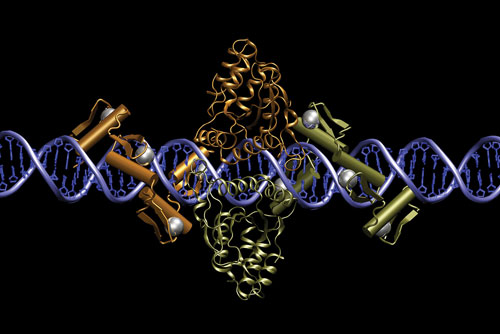
Two ZFNs bound to DNA [Jeff Miller, Sangamo BioSciences]
Transfecting New Genes Into the Liver
In the mid-80s, a six-year-old girl with familial hypercholesterolemia (FH) was given a liver transplant, planting a seed in the mind of James Wilson, M.D., Ph.D., “that if you replaced the LDL receptor in the liver, that you could correct the systemic metabolic defect in hypercholesterolemia.” He worked for years on ex vivo gene therapy using retrovirus and another 10 years on adenovirus before realizing that while that vector could transfer genes to the liver, it was extremely toxic “and we could not engineer the virus to avoid significant toxicity.”
By this time AAV—which didn’t elicit immune responses or inflammation toxicity—was being developed for in vivo gene therapy, but “only 1–2% of the liver cells took the gene up”—too little to correct diseases like homozygous FH, recalled Dr. Wilson, by now at the University of Pennsylvania, where he is currently a professor in the department of pathology and laboratory medicine, and the director of the gene therapy program. He is also the editor of Human Gene Therapy, a peer-reviewed journal published by Mary Ann Liebert, Inc.
Dr. Wilson used PCR to find new AAV isolates from humans and nonhuman primate genomes, many of which were 100 times more efficient than the original isolates, with AAV8 being the “most attractive for targeting liver.”
Using sophisticated mouse models of homozygous FH, Dr. Wilson’s work has progressed to late preclinical stages: “We’ve had a pre-IND meeting with FDA. We’re just completing the toxicology experiments, and hope to move into the clinic sometime in the next year,” Dr. Wilson noted. A recent Phase I study by another group using AAV8 to express Factor IX in hemophiliacs “has further encouraged us that AAV8 will be useful in targeting human liver by transfecting new genes into the hepatocytes.”
AAV8, a second-generation AAV technology, was discovered in James Wilson’s lab at UPenn.