April 15, 2013 (Vol. 33, No. 8)
Caitlin Smith
Recent years have seen an explosion of disease-relevant research on G-protein coupled receptors (GPCRs). Hot topics include strategies for targeting GPCRs therapeutically, and understanding the mechanisms of biased agonism. A number of distinguished speakers will present their latest GPCR research at the GPCR Colloquium at the “American Society for Pharmacology and Experimental Therapeutics” meeting.
In the phenomenon of biased agonism in GPCRs, a biased ligand activates one signaling pathway without activating another. “Biased agonism represented a paradigm shift,” says Robert Lefkowitz, M.D., professor of chemistry at Duke University and winner of the 2012 Nobel Prize in Chemistry with his colleague and former post-doc Brian Kobilka of Stanford University for their seminal work on 7-transmembrane domain GPCRs.
“Much to our total surprise, we realized that an agonist could stimulate one pathway—G proteins or the arrestins—without stimulating the other. It was a realization that this system could not only turn off G protein signaling, but also establish signaling pathways on its own.”
In addition to the development of GPCR research and biased agonism, Dr. Lefkowitz also plans to unveil some new results of a collaboration with Kobilka’s lab, in which they are trying to work out the molecular mechanisms of biased agonists. “We’re using a variety of structural approaches, including x-ray crystallography, to get at the mechanisms of biased agonists.”
Indeed, the importance of biased agonism in GPCR drug discovery is the work of one of Dr. Lefkowitz’ former post-docs, Jonathan Violin, Ph.D., now head of biology at Trevena. He will discuss how Trevena is using receptor bias for clinical development of pain therapeutics. They are focused on using biased ligands to separate “on-target adverse effects,” or adverse effects presumed inseparable from a drug’s pharmacology, from the drug’s intended therapeutic effects.
For example, Trevena recently discovered an analgesic drug targeting the mu-opioid receptor whose signaling mechanism partly resembles that of morphine, yet differs in that it does not engage beta-arrestins—and therapeutically shows reduced adverse effects of respiratory suppression and opioid-induced constipation.
“We are engaging the very well precedented and very valuable analgesia of this target, but hopefully in a safer and more tolerable fashion, by more precisely tuning in the kinds of intracellular signals that we desire,” says Dr. Violin.
He notes the value of beginning with known targets and signaling mechanisms, and then working to understand the mechanisms of biased ligands of these targets. “What we think is happening with biased ligands is that we are stabilizing a subset of conformations associated with the active pharmacological entity or entities,” he says. In other words, a biased ligand activates only a subset of the different signaling pathways and in vivo pharmacological responses that they normally observe with the full agonist.
“To us, that’s part of the value in our approach,” he says, “that we can take targets for which we know a lot about their clinical benefits or clinical risks, and dissect those so that we don’t have to lay out completely new biological pathways.”
“We’re interested in studying new, functionally selective molecules that will activate G protein pathways selectively, or activate the beta-arrestin pathways selectively,” says Jeff Aubé, Ph.D., professor and chemist at the University of Kansas. His work is motivated by the need to grow the toolbox of biased ligands.
“We’ve sought to expand the scope of available compounds for study in this field by using different approaches, including screening and de novo design,” he says. “We have identified preliminary examples of five new, entirely different chemical classes with a range of potencies, and qualitatively different pharmacologies.”
Dr. Aubé hopes that expanding the toolkit of biased ligands will help other researchers in the field. “There are a lot of people who are interested in indications like addiction, who would be interested in, say, a potent partial agonist,” he says. “But that’s not really available right now.”
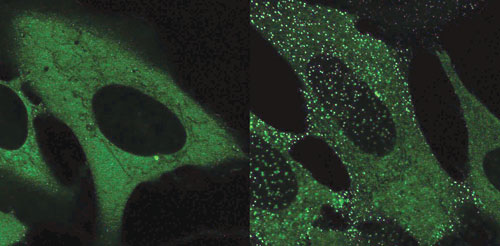
Beta-arrestin-2 tagged with GFP migrates from a cytosolic distribution in unstimulated Kappa Opioid Receptor-expressing cells (left) to associating with the membrane-bound receptors upon treatment with standard kappa opioid receptor agonists (right). [University of Kansas]
GPCRs in Therapeutics
“It is increasingly obvious that taking advantage of ligand-biased signaling will provide for some GPCR targets a way to modulate therapeutically relevant pathways while potentially avoiding unwanted physiology,” says Christian Felder, Ph.D., a research fellow in psychiatric disorders at Eli Lilly.
“Allosteric regulation of GPCRs has taken the science to a new level of possibilities, although with inherently increased complexity in execution.” He stresses the need for more effective pharmacological tools, which will entail further work on GPCR crystal structures, in silico molecular dynamic simulations, and translational bioassay development. “Without good ligand tools, research challenges such as deorphanizing of new GPCR targets and deconvoluting disease etiology become even bigger.”
Dr. Felder also believes that GPCR drug discovery will continue to benefit from partnerships among academia, government, and industry. “A deeper understanding of structure, function, and physiology can only happen when we bring together the various disciplines of chemical, physical, and biological sciences to embrace the obvious complexity of how GPCRs regulate complex pathways and circuits,” says Dr. Felder.
“Recent advances in active-state GPCR crystallography and in silico molecular dynamics are informing ligand-receptor interactions in much more detail,” resulting in more efficient drug design. Int vitro models, such as inducible pluripotent stem cells, can give relevant information in a disease context, which can in turn “inform translational animal models that may more directly mimic human disease etiology,” says Dr. Felder.
Heptares Therapeutics takes another angle on therapeutics, developing drugs to GPCR targets to which previous attempts have been unsuccessful, yet for which there is strong evidence for disease involvement. “There remain a large number of GPCRs with a high level of clinical validation in disease that have not been drugged by small molecules,” says the firm’s CSO, Fiona Marshall, Ph.D. “For example, GLP1 is an important target in diabetes. However, only injectable peptides have been discovered for this receptor so far.”
Heptares uses a structure-based drug design platform called StaR, which engineers GPCRs to increase their thermostability—the result being that they can be purified from cell membranes. This lets them take advantage of drug discovery methods commonly used for soluble proteins, but normally impossible with membrane proteins, such as x-ray crystallography.
“StaRs are locked in specific chosen conformational states, such as agonist or antagonist,” says Dr. Marshall, “and can be used to define the pharmacology of compounds by measuring the relative binding to different conformations—a process known as ‘reverse pharmacology’.”
Heptares uses x-ray structures to look at receptor binding sites and protein-ligand interactions. They utilize the atomic resolution of x-ray structures to find small but significant differences between ligand binding sites of GPCRs in activated and inactive states, and then use the protein structure for the form of their chosen target for drug discovery.
In her presentation, Dr. Marshall will discuss Heptares’ identification of drug candidates, including “the identification of highly selective muscarinic agonists for the treatment of Alzheimer’s disease, and the identification of orexin antagonists for sleep disorders and addiction,” she says. “I will also be giving a first look at the first Family B GPCR structure that has been solved.”
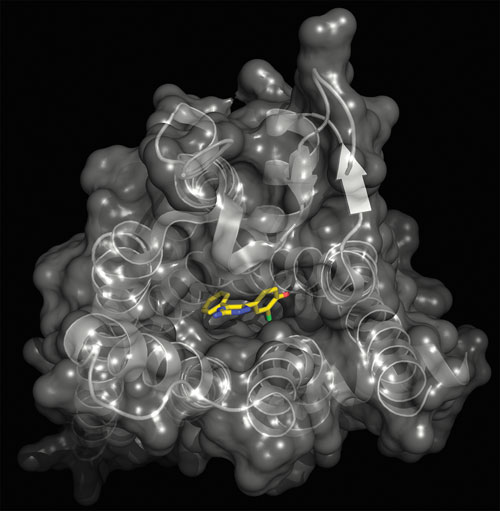
Surface of the Adenosine A2A StaR thermostabilized in the antagonist conformation, complexed with a synthetic antagonist. [Heptares Therapeutics]
GPCR Trafficking
Looking at therapeutic opportunities of GPCRs from another angle is the lab of Mark von Zastrow, M.D., Ph.D., professor of psychiatry and pharmacology at UCSF. Traditionally, GPCR trafficking can determine in part whether a signaling response is sustained or downregulated, and it occurs over a longer period of hours or more. But Dr. von Zastrow is looking at GPCR trafficking events that occur seconds to minutes after ligand application—an acute trafficking response that occurs much faster than previously thought.
“Such effects are much less well understood,” he says. “GPCR trafficking mechanisms offer, in principle, a wide range of new biochemical targets for therapeutic manipulation. To my knowledge, the in vivo potential of such targets remains a little-explored area.”
Dr. von Zastrow will discuss results on mechanisms of GPCR localization, trafficking, and signaling from both biochemical and optimal imaging techniques, and will focus on recent progress toward developing new therapeutics. “We are particularly interested in processes that affect neural and cardiovascular function,” he says. “An over-arching challenge is to link mechanistic understanding, elucidated largely in vitro or using reduced cell culture preparations, to in vivo effects as they occur in relevant tissues.”
The field is accumulating evidence for independent mechanisms of GPCR trafficking and GPCR signaling, according to Dr. von Zastrow. “The idea that drugs can selectively influence one of these was considered highly controversial even five years ago,” he says. “However, little is known about the consequences of such selective ligand effects in vivo, or their potential therapeutic significance. In my opinion, this represents another exciting frontier with great therapeutic potential.”